Virtsankarkailu (naiset)
Miten viitata Käypä hoito -suositukseen? «K1»1
Keskeinen sisältö
- Diagnostiikka tähtää virtsankarkailun tyypin (ponnistus-, pakko-, sekamuotoinen- tai
ylivuotovirtsankarkailu) ja haitta-asteen määrittämiseen.
- Määritys perustuu anamneesiin, kyselylomakkeisiin (ks. kappale Kyselylomakkeet «A1»2) sekä yleiseen ja gynekologiseen tutkimukseen yskäisytesteineen (ks. kaavio «Naisten virtsankarkailun selvittely avoterveydenhuollossa»1).
- Virtsankarkailun tyyppiä voi arvioida karkeasti kahdella avainkysymyksellä:
- Karkaako virtsa äkillisen ponnistamisen, yskäisyn tai aivastamisen yhteydessä?
- Myönteinen vastaus viittaa ponnistusvirtsankarkailuun.
- Onko sinulla voimakasta virtsaamistarvetta siten, että virtsa karkaa ennen kuin ehdit
WC:hen?
- Myönteinen vastaus viittaa pakkovirtsankarkailuun.
- Karkaako virtsa äkillisen ponnistamisen, yskäisyn tai aivastamisen yhteydessä?
- Painonhallinta, tupakoimattomuus, lantionpohjan lihaskunnon ylläpito, ummetuksen hoito ja erityisesti 65 vuotta täyttäneillä fyysinen aktiivisuus ehkäisevät virtsankarkailua.
- Virtsankarkailuoireita voidaan hoitaa useilla tavoilla. Hoidon valinnassa tulee huomioida
virtsankarkailun tyyppi, oireiden vakavuus ja hoidon yksilöllinen soveltuvuus (esim.
ikä, ylipaino):
- Painonpudotus voi vähentää ylipainoisten (ainakin keski-ikäisten ja nuorempien naisten) virtsankarkailua merkittävästi.
- Lantionpohjan lihasharjoittelu on usein riittävä hoito lievään ja keskivaikeaan ponnistusvirtsankarkailuun. Se edellyttää kuitenkin säännöllistä ja pitkäaikaista sitoutumista omatoimiseen harjoitteluun.
- Nauhaleikkaus on tehokas hoito vaikeaan ponnistusvirtsankarkailuun. Oireet häviävät kokonaan suurimmalla osalla potilaista.
- Täyteainepistokset (polyakryyliamidihydrogeeli) ovat vähemmän kajoava hoito ponnistusvirtsankarkailuun, mutta hyöty on vähäisempi nauhaleikkaukseen verrattuna.
- Atrofisen limakalvon hoito emättimeen annosteltavalla paikallisella estrogeenilla saattaa lievittää vaihdevuosi-iän saavuttaneiden naisten pakkovirtsankarkailun oireita.
- Lääkehoito (beeta3-agonistit ja antikolinergit) vähentävät pakkovirtsankarkailua.
- Botuliinitoksiini A -pistokset virtsarakon tähystyksen yhteydessä vähentävät pakkovirtsankarkailua, ja niitä voi harkita, jos muusta hoidosta ei ole riittävää apua.
- Iäkkään virtsankarkailun yksilöllinen hoitosuunnitelma perustuu kokonaisvaltaiseen
arvioon, jossa huomioidaan toimintakyky, gerastenia, kognitio ja monisairastavuus.
- Iäkkään virtsankarkailun hoitoon soveltuvat erityisesti lääkkeettömät hoidot, kuten liikunta- ja toimintakyvyn ylläpito.
- Iäkkäiden hoidossa antikolinergien haitat ylittävät useimmiten hyödyt.
- Myös ylivuotovirtsankarkailun ja lääkeaineiden provosoiman virtsankarkailun mahdollisuus tulee muistaa.
- Mikäli perusterveydenhuollon toimet eivät tuota riittävää apua virtsankarkailuoireeseen, ohjataan potilas erikoissairaanhoitoon (kaavio «Naisten virtsankarkailun selvittely avoterveydenhuollossa»1).
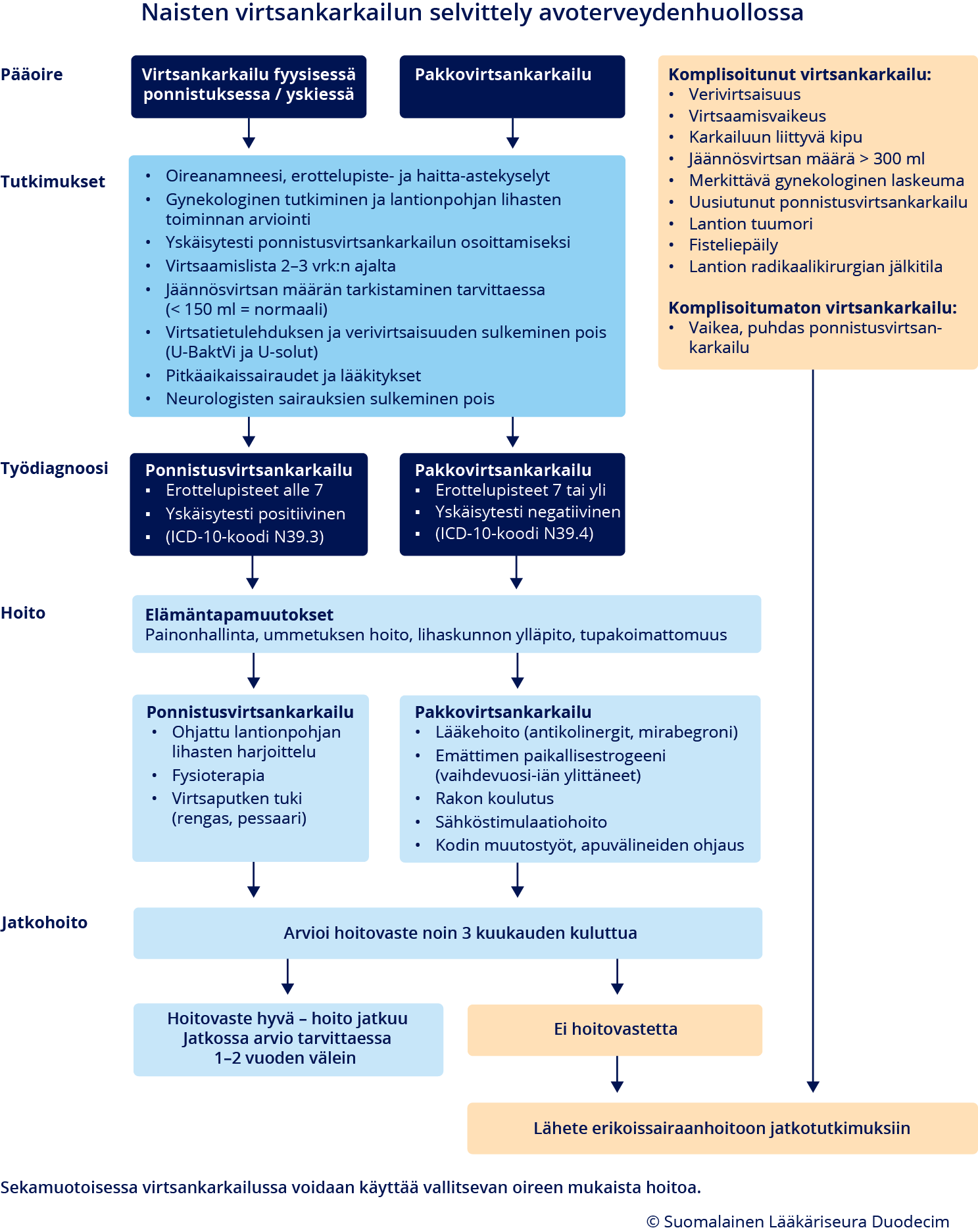
Naisten virtsankarkailun selvittely avoterveydenhuollossa
Suosituslauseet
Diagnostiikka «A6»3
|
Ehkäisy «A7»4
|
Hoito «A8»5
|
Iäkkäiden virtsankarkailun diagnostiikka ja hoito «A4»6
|
Tiivistelmä ja potilasversio
- Suosituksen tiivistelmä «Virtsankarkailu (naiset)»1
- Suosituksen yleiskielinen potilasversio suomeksi ja ruotsiksi (päivityksessä)
Tavoite
- Tavoitteena on tukea naisten virtsankarkailun eli virtsainkontinenssin tutkimus- ja hoitokäytäntöjä avoterveydenhuollossa ja erikoissairaanhoidossa.
Kohderyhmä
- Suosituksen kohderyhmänä ovat avoterveydenhuollon ja erikoissairaanhoidon lääkärit ja muu hoitohenkilökunta, kotihoito ja vanhusten hoitolaitosten henkilöstö sekä terveydenhuollon päätöksentekijät.
Määritelmä ja aiheen rajaus
- Virtsankarkailu tarkoittaa oireena mitä tahansa virtsan tahatonta karkailua. Oireiden,
löydösten ja tutkimusten pohjalta käytetään kansainvälistä luokittelua «Haylen BT, de Ridder D, Freeman RM, ym. An Interna...»1, joka on yhteneväinen ICD-10-luokituksen kanssa.
- Ponnistusvirtsankarkailu (stress urinary incontinence, SUI; ICD-10-koodi N39.3) on näkyvää fyysisen rasituksen, ponnistuksen, yskäisyn tai aivastuksen yhteydessä tapahtuvaa virtsan karkaamista.
- Pakkovirtsankarkailu (urgency urinary incontinence, UUI; ICD-10-koodi N39.4) on näkyvää virtsan karkaamista, johon liittyy samanaikainen äkillinen ja voimakas virtsaamistarve.
- Yliaktiivinen virtsarakko (overactive bladder) -termiä käytetään paljon virtsankarkailuun liittyvässä kirjallisuudessa. Se viittaa useimmiten virtsapakko-oireeseen, johon voi liittyä virtsankarkailua (wet overactive bladder).
- Sekamuotoisessa virtsankarkailussa (mixed urinary incontinence, MUI; ICD-10-koodi N39.4) esiintyy sekä ponnistus- että pakkovirtsankarkailua.
- Ylivuotovirtsankarkailu (overflow urinary incontinence; ICD-10-koodi R33) on virtsan karkaamista, joka liittyy virtsarakon akuuttiin tai krooniseen tyhjenemishäiriöön eli virtsaretentioon.
- Suositus koskee aikuisten naisten virtsankarkailua, joka aiheuttaa sosiaalista, hygieenistä tai muuta haittaa.
- Suosituksessa ei käsitellä virtsateiden anomalioista eikä fisteleistä johtuvaa virtsankarkailua.
- Kansainvälisten tiedejärjestöjen IUGA/ICS (International Urogynecological Association/International Continence Society) ylläpitämä termistö oireista ja löydöksistä kliiniseen ja tutkimuskäyttöön sisältää tarkemman kuvauksen virtsankarkailuun liittyvistä käsitteistä «Haylen BT, de Ridder D, Freeman RM, ym. An Interna...»1.
Esiintyvyys ja riskitekijät
Esiintyvyys
- Naisten virtsankarkailu on yleistä, ja se heikentää elämänlaatua. Tutkimuksissa virtsankarkailun
esiintyvyys vaihtelee suuresti virtsankarkailun määrittelyn ja tutkimusjoukon mukaan
«Hunskaar S, Burgio K, Diokno A, ym. Epidemiology a...»2, «Cerruto MA, D'Elia C, Aloisi A, ym. Prevalence, in...»3, «Schreiber Pedersen L, Lose G, Høybye MT, ym. Preva...»4.
- Norjalaisessa väestöpohjaisessa tutkimuksessa 25 %:lla naisista esiintyi jonkinlaista virtsankarkailua ja 7 %:lla siitä oli huomattavaa haittaa «Hannestad YS, Rortveit G, Sandvik H, ym. A communi...»5.
- Iän myötä virtsankarkailu lisääntyy (kuva «Naisten virtsankarkailun esiintyvyys ja ikä»2), «Hannestad YS, Rortveit G, Sandvik H, ym. A communi...»5, «Jahanlu D, Hunskaar S. The Hordaland Women's Cohor...»6, «Rortveit G, Hannestad YS, Daltveit AK, ym. Age- an...»7, «Matthews CA, Whitehead WE, Townsend MK, ym. Risk f...»8.
- Iäkkäiden virtsankarkailun on todettu olevan yhteydessä heikentyneeseen toiminta- ja liikuntakykyyn ja moniin pitkäaikaisiin sairauksiin «Maggi S, Minicuci N, Langlois J, ym. Prevalence ra...»9, «Ostaszkiewicz J, Johnston L, Roe B. Timed voiding ...»10.
- Virtsankarkailu voi olla myös ohimenevää. Vuosittaisen spontaanin paranemisen todennäköisyys vaihtelee 6 ja 38 %:n välillä «Hunskaar S, Burgio K, Diokno A, ym. Epidemiology a...»2, «Buckley BS, Lapitan MC, Epidemiology Committee of ...»11, «Jahanlu D, Hunskaar S. The Hordaland Women's Cohor...»6, «Wennberg AL, Molander U, Fall M, ym. A longitudina...»12.
- Virtsankarkailusta kärsivistä naisista vain osa hakee apua vaivaansa.

Naisten virtsankarkailun esiintyvyys ja ikä yli 20-vuotiailla naisilla.
Lähde: Rortveit G, Hannestad YS, Daltveit AK ym. Age- and type-dependent effects of parity on urinary incontinence: the Norwegian EPINCONT study. Obstet Gynecol 2001;98:1004-10
Riskitekijät
- Virtsankarkailu on yhteydessä useisiin riskitekijöihin. Kaikkien kliininen merkitys ei kuitenkaan ole selkeä.
- Keskeisiä riskitekijöitä ovat ikä «Naisten virtsankarkailun esiintyvyys ja ikä»2, ylipaino «Naisten virtsankarkailun esiintyvyys ja painoindeksi»3, diabetes, synnytykset ja kohdunpoisto «Sundqvist C, Li X, Sundquist K, ym. Sociodemograph...»13, «Abufaraj M, Xu T, Cao C, ym. Prevalence and trends...»14, «Shang X, Fu Y, Jin X, ym. Association of overweigh...»15, «Choi JM, Jiang J, Chang J, ym. Impact of Lifetime ...»16, «Hagen S, Sellers C, Elders A, ym. Urinary incontin...»17, «Wesnes SL, Hunskaar S, Bo K, ym. The effect of uri...»18.
- Diabetesta sairastavilla naisilla on suurentunut pakko- ja sekamuotoisen virtsankarkailun riski ja virtsankarkailu on usein vaikeampaa kuin diabetesta sairastamattomilla «Ebbesen MH, Hannestad YS, Midthjell K, ym. Diabete...»19, «Danforth KN, Townsend MK, Curhan GC, ym. Type 2 di...»20, «Løwenstein E, Jepsen R, Andersen LL, ym. Prevalenc...»21.
- Tanskalaisessa tutkimuksessa synnyttämättömistä naisista (keski-ikä 46 vuotta) virtsankarkailua esiintyi noin 10 %:lla, keisarileikkauksella synnyttäneistä 16 %:lla ja alateitse synnyttäneistä 21 %:lla «Rortveit G, Daltveit AK, Hannestad YS, ym. Urinary...»22. Systemaattisessa katsauksessa ja meta-analyysissä ponnistusvirtsankarkailua esiintyi 8 % enemmän alateitse synnyttäneillä verrattuna keisarileikkauksella synnyttäneisiin «Tähtinen RM, Cartwright R, Tsui JF, ym. Long-term ...»23, «Rortveit G, Daltveit AK, Hannestad YS, ym. Urinary...»22.
- Kohdunpoiston jälkeen virtsankarkailua esiintyy uutena oireena 8,5–15,4 %:lla riippumatta
leikkauksen aiheesta «Humalajärvi N, Aukee P, Kairaluoma MV, ym. Quality...»24, «Christoffersen NM, Klarskov N, Gradel KO, ym. Incr...»25.
- Kohdunpoisto laskeuman takia saattaa kuitenkin vähentää virtsankarkailua ja tiheävirtsaisuutta «Humalajärvi N, Aukee P, Kairaluoma MV, ym. Quality...»24.
- Myös ummetus lisää virtsankarkailuoireiden riskiä «Bardino M, Di Martino M, Ricci E, ym. Frequency an...»26, «Koskimäki J, Hakama M, Huhtala H, ym. Association ...»27.
- Selkäkipu ja lantiorenkaan kipu lisäävät virtsankarkailun riskiä «Bertuit J, Bakker E, Rejano-Campo M. Relationship ...»28, «Welk B, Baverstock R. Is there a link between back...»29.
- Elintavat voivat vaikuttaa virtsankarkailuoireeseen.
- Liiallinen nesteiden nauttiminen lisää virtsaamistarvetta ja voi altistaa virtsankarkailulle «Townsend MK, Jura YH, Curhan GC, ym. Fluid intake ...»30, «Imamura M, Williams K, Wells M, ym. Lifestyle inte...»31. Tarvittava nestemäärä on normaalisti 1,5–2 litraa vuorokaudessa «Faiena I, Patel N, Parihar JS, ym. Conservative Ma...»32.
- Kofeiinilla ei ole merkittävää vaikutusta virtsankarkailuun «Jura YH, Townsend MK, Curhan GC, ym. Caffeine inta...»33, «Hirayama F, Lee AH. Green tea drinking is inversel...»34, «Sun S, Liu D, Jiao Z. Coffee and caffeine intake a...»35.
- Tupakointi lisää pakkovirtsankarkailun riskiä sekä virtsapakko-oireita ja tihentynyttä virtsaamistarvetta «Tähtinen RM, Auvinen A, Cartwright R, ym. Smoking ...»36, «Kawahara T, Ito H, Yao M, ym. Impact of smoking ha...»37, «Michel KF, Rangnekar AN, Slinger M, ym. Associatio...»38.
- Alkoholi toimii diureettina ja saattaa siten lisätä virtsankarkailua.
- Vähän liikkuvien virtsankarkailun riski on suurempi kuin pitkäaikaista kohtuullista
kuntoliikuntaa harrastavien «Townsend MK, Danforth KN, Rosner B, ym. Physical a...»39, «Kim MM, Ladi-Seyedian SS, Ginsberg DA, ym. The Ass...»40.
- Suomalaisista vaihdevuosi-ikäisistä vähän liikkuvista naisista virtsankarkailua on 43 %:lla ja paljon liikkuvista 32 %:lla «Laakkonen EK, Kulmala J, Aukee P, ym. Female repro...»41.
- Voimakkaat tai pitkäkestoiset ponnistukset ja rasitus urheilusuorituksen yhteydessä voivat aiheuttaa virtsan karkaamista, vaikkei virtsankarkailuoireita esiintyisi muissa tilanteissa.
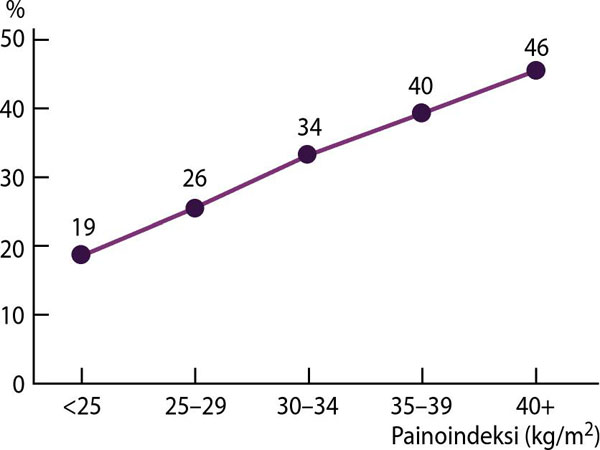
Naisten virtsankarkailun esiintyvyys ja painoindeksi yli 20-vuotiailla naisilla.
Lähde: Hannestad YS, Rortveit G, Daltveit AK ym. Are smoking and other lifestyle factors associated with female urinary incontinence? The Norwegian EPINCONT Study. BJOG 2003;110:247-54
Esiintyvyys neurologisten sairauksien yhteydessä
- Virtsankarkailua esiintyy useiden neurologisten sairauksien yhteydessä.
- Arviot esiintyvyydestä vaihtelevat tutkimuksittain, mikä johtunee siitä, että sairauden kesto on eri aineistoissa erilainen. Esimerkiksi muistisairauksissa, MS-taudissa, multippeliskleroosissa ja Parkinsonin taudissa oireet lisääntyvät sairauden edetessä.
- Keskushermostosairauksien, kuten aivoinfarktin, aivoverenvuodon ja muistisairauksien, virtsarakko-oireita ovat tihentynyt virtsaamistarve ja virtsankarkailu, sekä virtsarakon tyhjenemishäiriö (retentio) «Tibaek S, Gard G, Klarskov P, ym. Prevalence of lo...»42, «Sakakibara R, Uchiyama T, Yamanishi T, ym. Dementi...»43, «de Sèze M, Ruffion A, Denys P, ym. The neurogenic ...»44, «Li FF, Cui YS, Yan R, ym. Prevalence of lower urin...»45, «Ransmayr GN, Holliger S, Schletterer K, ym. Lower ...»46.
- Esiintyvyyttä on kuvattu tarkemmin lisätietoaineistossa «Virtsankarkailun esiintyvyys neurologisissa sairauksissa»1.
Diagnostiikka
- Diagnostiikan tavoitteena on määrittää virtsankarkailun tyyppi «Virtsankarkailun tyypit ja mekanismit»2, syy, haitta-aste ja vaikutus elämänlaatuun. Virtsankarkailun tyyppi vaikuttaa hoidon valintaan.
- Ks. kaavio avoterveydenhuollon diagnostiikasta ja hoidosta «Naisten virtsankarkailun selvittely avoterveydenhuollossa»1.
- Virtsankarkailun tyyppiä voi arvioida karkeasti kahdella avainkysymyksellä:
- Karkaako virtsa äkillisen ponnistamisen, yskäisyn tai aivastamisen yhteydessä?
- Myönteinen vastaus viittaa ponnistusvirtsankarkailuun.
- Onko sinulla voimakasta virtsaamistarvetta siten, että virtsa karkaa ennen kuin ehdit
WC:hen?
- Myönteinen vastaus viittaa pakkovirtsankarkailuun.
- Karkaako virtsa äkillisen ponnistamisen, yskäisyn tai aivastamisen yhteydessä?
- Katso iäkkäiden potilaiden diagnostiikan erityispiirteet tarkemmin kappaleesta Iäkkäiden virtsankarkailun diagnostiikka ja hoito «A4»6.
Anamneesi
- Virtsankarkailupotilaan anamneesiin sisältyy:
- pitkäaikaissairaudet ja -oireet (huomioi etenkin diabetes ja neurologiset sairaudet)
- lääkehoito (ks. taulukko «Virtsankarkailua mahdollisesti aiheuttavia tai pahentavia lääkeaineita, jotka on syytä huomioida erityisesti iäkkäiden hoidossa....»4)
- synnytysten lukumäärä ja synnytyskomplikaatiot (ks. kappale Riskitekijät «A2»7)
- synnytin- tai virtsaelinleikkaukset (mahdollinen sädehoito)
- kuukautiskierto (menopaussi)
- kaksi avainkysymystä virtsankarkailun tyypin arvioimiseksi (ks. edellä)
- virtsankarkailuoireiden alkaminen ja kesto
- äkillinen virtsatulehdus, joka voi olla uutena alkaneen virtsankarkailun taustalla «DuBeau CE, Kuchel GA, Johnson T 2nd, ym. Incontine...»47, «Schröder A, Abrams P, Andersson KE ym. Urinary inc...»48
- apuvälineiden (mm. kontinenssisuojat) käyttötarve (ks. kohta Apuvälineet ja hoitotarvikkeet «A3»8)
- elintavat (mm. juomisen määrä, tupakointi)
- iäkkään asuin- ja kotihoito-olot.
Kyselylomakkeet
Suositus: Ohjaa potilaat täyttämään erottelupiste- ja haitta-aste-lomakkeet ja virtsaamispäiväkirja.
- Avainkysymysten lisäksi virtsankarkailun tyyppiä voi arvioida tarkemmin erottelupistelomakkeella
(ks. erottelupistelomake «https://www.kaypahoito.fi/xmedia/ykt/inkontinenssi_erottelu.pdf»1 (PDF)), virtsaamispäiväkirjalla «hoi50050a.pdf»1 ja kliinisillä löydöksillä. Käy lomakkeiden vastaukset läpi potilaan kanssa vastaanotolla.
- Erottelupistemäärä alle 7 viittaa ponnistusvirtsankarkailuun. Mitä pienempi pistemäärä on, sitä todennäköisimmin kyseessä on puhdas ponnistusvirtsankarkailu «Klovning A, Hunskaar S, Eriksen BC. Validity of a ...»49.
- Erottelupistemäärä 7 tai yli viittaa sekamuotoiseen tai pakkovirtsankarkailuun.
- Virtsaamispäiväkirjan avulla arvioidaan virtsaamistiheys, virtsamäärät ja nautitut nestemäärät, ja se täytetään 2–3 vuorokauden ajalta. Katso tulkintaohjeet lisätietomateriaalista «Virtsaamispäiväkirja virtsaamishäiriöiden selvittelyssä ja hoidossa»3.
- Erottelupistelomakkeen ja virtsaamispäiväkirjan täyttäminen ennen ensimmäistä vastaanottokäyntiä helpottaa oireen tyypin ja vakavuuden arvioimista ja voi vähentää tarvittavien arviointikäyntien määrää.
- Virtsankarkailun haittaa voi arvioida
- haitta-astelomakkeella (ks. haitta-astelomake «https://www.terveysportti.fi/xmedia/ykt/inkontinenssi_haitta.pdf»2 (PDF))
- VAS-janalla (visual analogue scale 0–10) tai numeroasteikolla (NRS, numeric rating scale 0–10).
Kliininen tutkimus
- Kliinisessä tutkimuksessa selvitetään
- yleistila, liikuntakyky
- paino ja pituus (painoindeksi).
- Tarvittaessa tehdään jäännösvirtsan mittaus (kertakatetrointi tai ultraäänitutkimus).
- Ks. Lääkärin tietokantojen video Jäännösvirtsan mittaus (merkittävä virtsaretentio) «Jäännösvirtsan mittaus»1 (vaatii käyttöoikeuden) ja lisätietoa «Virtsarakon tilavuuden laskeminen sekä virtsateiden rakenteen ja toiminnan selvittely ultraäänitutkimuksella»4.
- Tutkimusta kannattaa harkita, jos potilas kertoo virtsaamisvaikeudesta ja rakko palpoituu «Nambiar AK, Arlandis S, Bø K, ym. European Associa...»50 tai jos potilaalla on laskeumia, diabetes, toistuvia virtsatietulehduksia, ummetusta, potilas on iäkäs tai hän käyttää keskushermostoon vaikuttavia lääkkeitä «Schröder A, Abrams P, Andersson KE ym. Urinary inc...»48.
- Seurantamittaus kannattaa tehdä, mikäli jäännösvirtsan määrä on suuri (yli 2–3 dl).
- Gynekologisessa perustutkimuksessa huomioidaan erityisesti
- arvio limakalvojen kunnosta (atrofia) ja laskeumista
- kohdun ja munasarjojen palpaatio alavatsan kasvainten ja virtsaretention pois sulkemiseksi
- yskäisytesti, ks. video «Yskäisytesti (video)»5
- Epäselvissä tapauksissa käytetään täydentäviä tutkimuksia (ks. alla).
- lantionpohjan lihasvoiman arviointi sormitestillä, ks. lisätietoaineisto «Lantionpohjan lihasten sormitestaus»6.
- Tarvittaessa selvitetään neurologinen status.
- Nopeasti alkaneen virtsankarkailun taustalla voi olla diagnosoimaton neurologinen sairaus.
Laboratoriotutkimukset
- Virtsankarkailun diagnostiikassa tarvitaan vain vähän laboratoriotutkimuksia.
- Mikäli oireet viittaavat virtsatieinfektioon (esimerkiksi äkillinen alku tai paheneminen, muut virtsatieinfektion oireet), harkitse mikrobilääkehoitoa. Virtsanäytteet saattavat tarkentaa diagnostiikkaa, mutta tulkinnassa kannattaa huomioida oireeton bakteriuria ja väärän negatiivisen tuloksen mahdollisuus. Ks. Käypä hoito -suositus Virtsatieinfektiot «Virtsatieinfektiot»3, «Virtsatieinfektiot. Käypä hoito -suositus. Suomala...»51.
- Erotusdiagnostiikassa voidaan käyttää virtsan partikkelilaskentaa rakkosyövän sulkemiseksi
pois.
- Satunnaista mikroskooppista verivirtsaisuutta voi ilmetä voimakkaan fyysisen rasituksen, yhdynnän, lievän vamman tai kuukautisvuodon johdosta.
- Makroskooppinen verivirtsaisuus tai yli 40-vuotiaalla toistuva mikroskooppinen verivirtsaisuus edellyttävät arviota jatkotutkimusten tarpeesta. Arviossa huomioidaan oireet (kipu tai infektiotyyppiset oireet ilman vakuuttavaa bakteerilöydöstä, lämpöily, niveloireet, ihottuma) ja rakkosyövän riskitekijät, kuten tupakointi ja kemikaalialtistus «Rife CC, Farrow GM, Utz DC. Urine cytology of tran...»52, «Koss LG, Deitch D, Ramanathan R, ym. Diagnostic va...»53, «Chahal R, Gogoi NK, Sundaram SK. Is it necessary t...»54. Ks. Lääkärin tietokantojen artikkeli Verivirtsaisuus «Verivirtsaisuus»2 (vaatii käyttöoikeuden).
Täydentävät tutkimukset
- Täydentäviä tutkimuksia ovat kystoskopia, urodynaamiset mittaukset, kuvantamistutkimukset
ja vaippatesti, joita käytetään tarvittaessa erikoissairaanhoidossa (ks. kaavio «Naisten virtsankarkailun selvittely avoterveydenhuollossa»1), kun
- esiintyy epätyypillisiä oireita (esim. virtsarakon tyhjenemisvaikeuksia, ylivuotovirtsankarkailua, rakon ärsytysoireita) tai oireet ovat alkaneet äkillisesti
- virtsankarkailun tyypin määrittäminen jää kliinisesti epävarmaksi
- virtsankarkailu on uusiutunut leikkaushoidon jälkeen
- epäillään neurologista sairautta
- epäillään virtsarakon sairautta (esim. rakon kipuoireyhtymä, rakkokivi tai -syöpä), alavatsan kasvainta (esim. munasarjakasvain, kookas myooma) tai fisteliä.
Kystoskopia
- Kystoskopian merkitys on ensisijaisesti erotusdiagnostinen «Kystoskopia virtsainkontinenssin diagnostiikassa»7.
- Kystoskopian aiheet ovat
- makroskooppinen verivirtsaisuus tai toistuva mikroskooppinen verivirtsaisuus (yli 5–15 punasolua näkökentässä; huomioitava paikallisen laboratorion viitearvot) hoitoon reagoimaton vaikea tiheävirtsaisuus tai virtsaamispakko-oire
- rakon toiminnallinen kapasiteetti alle 100–150 ml
- kipu virtsatessa tai rakkokipu
- epäily fistelistä, rakkovauriosta tai divertikkelistä.
Urodynaamiset mittaukset
- Urodynaamisia mittauksia käytetään, kun virtsankarkailun tyyppi jää kliinisissä perustutkimuksissa epäselväksi tai suunnitellaan uusiutuneen virtsankarkailun leikkaushoitoa «Urodynaamiset mittaukset naisen virtsainkontinenssin diagnostiikassa»8.
- Tutkimus koostuu neljästä osasta:
- virtsasuihkun virtausmittauksesta (flowmetria)
- siihen liitetystä jäännösvirtsan mittauksesta
- rakon painemittauksesta (kystometria)
- virtsaputken painemittauksesta.
- Tutkimusmenetelmät eivät ole standardoituja, ja ne vaihtelevat sairaaloittain, tutkijoittain ja laitteistoittain.
Kuvantamistutkimukset
- Ultraäänitutkimuksella voidaan määrittää jäännösvirtsan määrä, rakon tilavuus ja virtsankarkailuleikkauksen verkkonauhan sijainti, sulkea pois lantion alueen kasvaimia ja opettaa lantionpohjan lihasten hallintaa «Goode PS, Locher JL, Bryant RL, ym. Measurement of...»55, «Bernstein IT. The pelvic floor muscles: muscle thi...»56, «Dietz HP, Wilson PD, Clarke B. The use of perineal...»57, «Kociszewski J, Rautenberg O, Kuszka A, ym. Can we ...»58, «Haylen BT, Maher CF, Barber MD, ym. An Internation...»59. Ks. lisätietoaineisto «Virtsarakon tilavuuden laskeminen sekä virtsateiden rakenteen ja toiminnan selvittely ultraäänitutkimuksella»4.
- Virtsaputken kuvantaminen voidaan tehdä välilihan alueelta (perineaalinen ultraäänitutkimus) tai emättimen tai peräsuolen kautta «Tunn R, Schaer G, Peschers U, ym. Updated recommen...»60, «Virtanen HS, Kiilholma P. Urogynecologic ultrasoun...»61, «Dalpiaz O, Curti P. Role of perineal ultrasound in...»62.
- Magneettitutkimuksella saadaan tarkempaa diagnostiikkaa lantion sairauksista ja anatomisista muutoksista (mm. virtsaputken divertikkelit, fistelit) «Kirschner-Hermanns R, Fielding JR, Versi E, ym. Ma...»63, «Rinne K, Kainulainen S, Aukee S, ym. Dynamic MRI c...»64.
- Uretrokystografiaa (UCG) käytetään ensisijaisesti virtsarakon fistelidiagnostiikassa.
Vaippatesti
- Vaippatestin avulla voidaan selvittää ponnistusvirtsankarkailua sekä karkaavan kokonaisvirtsan määrää grammoissa «Gilleran JP, Zimmern P. An evidence-based approach...»65.
- Vaippatestiä käytetään lähinnä kliinisissä tutkimuksissa, ja sen käyttö ja merkitys potilastyössä on vähäinen.
Ehkäisy
Suositus: Tarjoa raskaana olevalle ja synnyttäneelle neuvolassa ohjeistusta lantionpohjan lihasharjoittelusta.
- Lantionpohjan lihasharjoittelu raskauden aikana todennäköisesti ehkäisee virtsankarkailua raskauden aikana ja synnytyksen jälkeen «Pelvic muscle training before giving birth likely decreases urinary incontinence episodes both during the pregnancy and postpartum.»B.
- Lantionpohjan lihasharjoittelu synnytyksen jälkeen saattaa vähentää virtsankarkailuoireita «Pelvic floor muscle training during the postpartum period may decrease urinary incontinence episodes.»C.
- Lantionpohjan lihasten tunnistamisen ja harjoitukset voi ohjata terveydenhuollon ammattilainen. Ks. lisätietoaineisto «Lantionpohjan lihasten harjoitteluohje»9.
- Virtsankarkailua voidaan ehkäistä painonhallinnalla, tupakoimattomuudella, lihaskunnon ylläpidolla ja ummetuksen hoidolla. Ks. Käypä hoito -suositukset Lihavuus (lapset, nuoret ja aikuiset) «Lihavuus (lapset, nuoret ja aikuiset)»4, «Lihavuus (lapset, nuoret ja aikuiset). Käypä hoito...»66 ja Tupakka- ja nikotiiniriippuvuuden ehkäisy ja hoito «Tupakka- ja nikotiiniriippuvuuden ehkäisy ja hoito»5, «Tupakka- ja nikotiiniriippuvuuden ehkäisy ja hoito...»67.
- Lantionpohjan lihasvoiman lisääminen vaatii säännöllistä harjoittelua (ks. harjoitteluohje lisätietomateriaalista «Lantionpohjan lihasten harjoitteluohje»9).
- Alatiesynnytyksen hyvä hoito (välilihan tukeminen ja ponnistusvaiheen pitkittymisen välttäminen ja välilihan leikkaaminen tarvittaessa) saattaa myös ehkäistä virtsankarkailua «Linneberg S, Leenskjold S, Glavind K. A five year ...»68, «Brown SJ, Gartland D, Donath S, ym. Effects of pro...»69, «Leenskjold S, Høj L, Pirhonen J. Manual protection...»70, «Jiang H, Qian X, Carroli G, ym. Selective versus r...»71, «Okeahialam NA, Sultan AH, Thakar R. The prevention...»72.
Hoito
Suositus: Suosittele ylipainoiselle virtsankarkailusta kärsivälle potilaalle painonpudotusta ja järjestä siihen tarvittavat tukitoimet.
- Laihduttaminen todennäköisesti vähentää ylipainoisten naisten virtsankarkailua «Weight loss likely decreases urinary incontinence episodes.»B.
- Ks. lisätietoa Lihavuus (lapset, nuoret ja aikuiset) Käypä hoito -suosituksesta «Lihavuus (lapset, nuoret ja aikuiset)»4, «Lihavuus (lapset, nuoret ja aikuiset). Käypä hoito...»66.
- Hoidon suunnittelussa otetaan huomioon virtsankarkailun tyyppi, oireiden vaikeusaste ja potilaan toiveet.
Elintapamuutokset
- Jo 5–10 %:n painonpudotus voi vähentää virtsankarkailua merkittävästi (taulukko «Pakkovirtsankarkailun hoitovaihtoehdot ja virtsankarkailukertojen määrä 8–12 viikon seurannassa....»2).
- Iäkkäiden osalta ks. tarkemmin kappaleesta Iäkkäiden virtsankarkailun diagnostiikka ja hoito «A4»6.
- Tupakoivilla on tupakoimattomia enemmän virtsankarkailua «Hannestad YS, Rortveit G, Daltveit AK, ym. Are smo...»73, «Tähtinen RM, Auvinen A, Cartwright R, ym. Smoking ...»36. Ks. Käypä hoito -suositus Tupakka- ja nikotiiniriippuvuuden ehkäisy ja hoito «Tupakka- ja nikotiiniriippuvuuden ehkäisy ja hoito»5, «Tupakka- ja nikotiiniriippuvuuden ehkäisy ja hoito...»67.
- Liiallinen nesteiden nauttiminen ja alkoholi lisäävät virtsaneritystä.
- Rakkokoulutuksella pyritään pidentämään tiheää virtsaamisväliä ja parantamaan virtsanpidätyskykyä. Tutkimusnäyttö rakkokoulutuksen hyödyistä oireiden vähentämiseksi on hyvin epävarmaa «The evidence on bladder training to treat incontinence symptoms is very uncertain.»D, «Wallace SA, Roe B, Williams K, ym. Bladder trainin...»74. Ks. myös lisätietoaineiston potilasohje «Virtsarakon kouluttaminen, potilasohje»10.
- Ummetus saattaa lisätä virtsankarkailuoireita, joten sen ehkäisy ja hoito on syytä huomioida «Füsgen I, Wiedemann A. [Chronic Constipation: A Ge...»75.
Lihasharjoittelu
- Lantionpohjan ohjeistettu lihasharjoittelu todennäköisesti vähentää virtsankarkailua
ponnistusvirtsankarkailussa ja saattaa vähentää myös muun tyyppistä virtsankarkailua
«Pelvic floor muscle exercise likely decreases the urinary incontinence symptoms.»B.
- Lihasharjoittelu on usein riittävä hoito lievässä ja keskivaikeassa ponnistusvirtsankarkailussa. Vaikeat oireet vaativat useimmiten kajoavaa hoitoa.
- Lantionpohjan lihasten tunnistamisen ja harjoittelun voi ohjata asiaan perehtynyt
terveydenhuollon ammattilainen (ks. lisätietoa sormitestaus «Lantionpohjan lihasten sormitestaus»6, harjoitteluohje «Lantionpohjan lihasten harjoitteluohje»9).
- Jos lihasten tunnistaminen ja harjoittaminen eivät onnistu, potilas tulisi ohjata lantionpohjan fysioterapiaan. Ks. lisätietoaineisto «Fysioterapia virtsankarkailun hoidossa»11.
- Tutkimusnäyttö biopalautteen hyödyistä lihasharjoittelussa on hyvin epävarmaa «The evidence on Pelvic Floor Muscle Training (PFMT) with EMG Biofeedback (EMG-BF) is very uncertain.»D, mutta se voi auttaa tunnistamaan lantionpohjan lihakset.
- Vaikuttava lihasharjoittelu edellyttää sitoutumista säännölliseen ja pysyvään harjoitteluun.
- Huonon fysioterapiatuloksen ennustetekijöinä saattavat olla vaikeaksi koettu virtsankarkailu, painoindeksi > 30 kg/m2 (ks. kohta Elintapamuutokset «A5»9), aikaisemman fysioterapian huono tulos ja heikko psyykkinen ja fyysinen terveydentila «Hendriks EJ, Kessels AG, de Vet HC, ym. Prognostic...»76.
- Mobiilisovellukset saattavat auttaa lihasharjoitteluun sitoutumisessa ja näin parantaa hoidon tuloksia «Hou Y, Feng S, Tong B, ym. Effect of pelvic floor ...»77, «de Araujo CC, Brito LGO, Marques AA, ym. Use of a ...»78, «Wadensten T, Nyström E, Franzén K, ym. A Mobile Ap...»79. Eri sovellusten hyödyt voivat vaihdella.
Estrogeenihoito
- Emättimeen annosteltava paikallinen estrogeenihoito saattaa lievittää vaihdevuosi-iän
ylittäneiden naisten virtsankarkailuoireita «Topical estrogen therapy may reduce urinary incontinence symptoms.»C.
- Paikallinen estrogeenihoito todennäköisesti vähentää virtsatietulehduksia «Vaginal oestrogens appear to be effective for reducing recurrent urinary tract infections compared to placebo in postmenopausal women.»B ja saattaa vähentää virtsarakon ärsytysoireita, tiheävirtsaisuutta, yövirtsaisuutta ja virtsankarkailua «Cody JD, Jacobs ML, Richardson K, ym. Oestrogen th...»80, «Ewies AA, Alfhaily F. Topical vaginal estrogen the...»81, «Cardozo L, Lose G, McClish D, ym. A systematic rev...»82, «Rahn DD, Carberry C, Sanses TV, ym. Vaginal estrog...»83, «Te West NID, Harris K, Jeffrey S, ym. The effect o...»84, «Nemirovsky A, Villela NA, Yuan JC, ym. Vaginal Hor...»85, «Collà Ruvolo C, Gabrielli O, Formisano C, ym. Pras...»86, «Ren C, Qiang Z. Topical estrogen therapy ameliorat...»87.
- Rintasyövän sairastaneen naisen paikallishoitoon ei ole estettä «McVicker L, Labeit AM, Coupland CAC, ym. Vaginal E...»88, «Tiitinen A, Kero K. Paikallisestrogeenit ja rintas...»89. Ks. Käypä hoito -suositus Vaihdevuodet «Vaihdevuodet»6, «Vaihdevuodet. Käypä hoito -suositus. Suomalaisen L...»90.
- Systeeminen hoito ei lievitä virtsankarkailuoireita vaan saattaa jopa hieman pahentaa niitä «Rahkola-Soisalo P, Savolainen-Peltonen H, Gissler ...»91.
Muut hoidot
- Sähköstimulaatiota voidaan antaa kotona tai polikliinisesti.
- Säärihermon sähköstimulaatiohoito todennäköisesti vähentää pakkovirtsankarkailua «Percutaneous Tibial nerve stimulation (PTNS) likely decreases overactive bladder symptoms slightly.»B.
- Kotisähkölaitteita (TNS, TENS, EMS, NMES) voi käyttää ponnistus, pakko- ja sekamuotoisen virtsankarkailun hoidossa «Kotona toteutettava sähköhoito virtsankarkailun hoidossa»12.
- Emättimeen annosteltava prasteroni saattaa lievittää virtsankarkailuoireita, mutta tutkimusnäyttö on vielä vähäistä «Pautasso S, Mancarella M, Novara L, ym. Intravagin...»92, «Misasi G, Russo E, Montt Guevara MM, ym. Effects o...»93, «Collà Ruvolo C, Ursino M, Formisano C, ym. Urodyna...»94, «Rubin R, Sanaee M, Yee A, ym. Prevalence of urinar...»95.
- Tutkimusnäyttö akupunktion vaikutuksista on hyvin epävarmaa «The evidence on acupuncture for urinary incontinence symptoms is uncertain.»D.
Pakkovirtsankarkailun hoito
Suositus: Harkitse potilaan kanssa lääkehoitoa huomioiden oireiden vaikeusaste ja lääkehoidon rajallinen vaikutus.
- Potilaat, joilla on enemmän oireita, saavat lääkehoidosta todennäköisesti suuremman hyödyn.
Suositus: Arvioi virtsankarkailun tilanne 2–3 kuukauden kuluttua lääkehoidon aloituksesta ja lääkehoidon jatkuessa ja hoidon muutosten tarve 1–2 vuoden välein.
- Hoidon riittävyyden ja tarpeellisuuden arvioimiseen ei useimmiten tarvita erillistä vastaanottokäyntiä.
- Hoidon vaikutus lienee luonteeltaan oireita vähentävä (ei oireet poistavaa), ja mikäli potilas onkin seurannassa oireeton, lääkityksen voi koettaa purkaa.
- Mikäli potilaalla on seurannassa häiritsevät oireet, mieti, voiko hoitoa tehostaa
tai vaihtaa (huomioi myös lääkkeetön hoito) ja ohjaa potilas tarvittaessa erikoissairaanhoidon
arvioon.
- Lääkehoidoksi voi kokeilla tarvittaessa toisen lääkeryhmän lääkettä tai antikolinergin ja beeta3-agonistin yhdistelmää «Dey A, Georgiadis G, Umezurike J, ym. Mirabegron V...»96.
- Termiä yliaktiivinen virtsarakko (overactive bladder) käytetään paljon virtsankarkailuun liittyvässä kirjallisuudessa. Se viittaa useimmiten virtsapakko-oireeseen, johon voi liittyä virtsankarkailua (wet overactive bladder).
Lääkehoito
- Pakkovirtsankarkailun lääkehoidon voi toteuttaa perusterveydenhuollossa. Mahdolliset hoitovaihtoehdot ja niihin liittyvät tyypilliset hyödyt ja haitat on esitetty alla olevassa taulukossa «Pakkovirtsankarkailun hoitovaihtoehdot ja virtsankarkailukertojen määrä 8–12 viikon seurannassa....»2.
- Myös sekamuotoisen virtsankarkailun hoidossa voidaan käyttää lääkehoitoa, erityisesti jos pakkovirtsankarkailu on vallitseva oire.
| Hoito | Virtsankarkailukertojen väheneminen (per 24 t) [näytönaste]* | Yleiset haitat – lääkkeen vuoksi haitan saavien potilaiden osuus (riskiero)*** | Kommentit |
|---|---|---|---|
| * Hyöty kuvaa suhteellista virtsankarkailukertojen vähenemää. Keskimääräinen absoluuttinen
hoitovaikutus vaihtelee potilaan lähtötason ja oireiden luonnollisen kulun mukaan.
Myös lääkkeen hoitovaikutuksessa saattaa olla yksilöllisiä eroja. ** Esimerkiksi jos potilaan virtsankarkailu vähenee seurannassa 20 % ilman lääkehoitoa, beeta3-agonistilääkitys huomioiden virtsankarkailu vähentyisi 42 %. Virtsankarkailun väheneminen seurannassa = Lähtötaso – kipu seurannassa ilman hoitoa x hoitovaikutus = 1 – 0,8 x 0,72 = 0,42. *** Riskiero (risk difference) lumeeseen / hoitamatta jättämiseen verrattuna. Todellisuudessa haittaa saa useampi, koska moni saa haittatapahtuman myös ilman hoitoa ja kyseinen oire saattaa lääkkeen vuoksi pahentua. Myös haittavaikutusten riski voi vaihdella potilaan ominaisuuksien mukaan. Hyöty ja haitta -taulukoita varten arvioimme hoitojen suhteellista hyötyä verrattuna hoitamatta jättämiseen. Menetelmät on kuvattu lisätietomateriaalissa «Calculation of relative mean difference»13. |
|||
| Oireiden luonnollinen kulku «Irwin DE, Milsom I, Chancellor MB, ym. Dynamic pro...»97 vaihtelee huomattavasti yksilöiden välillä, ja lääkevaikutuksissakin saattaa olla yksilöllisiä eroja. Keskimäärin oireet vähenevät seurannassa myös ilman hoitoa, minkä vuoksi lääkevaikutuksen erottaminen oireiden luonnollisesta kulusta voi olla vaikeaa «Khullar V, Rahnama'i MS, Veit-Rubin N, ym. Can we ...»98.** | |||
| Perusterveydenhuolto | |||
| Beeta3-agonistit | -28 % (-0,44 kertaa) «Mirabegron probably decreases incontinence episodes slightly in patients with overactive bladder.»B | Vähäiset haitat | |
| Antikolinergit | -32 % (-0,48 kertaa) «Anticholinergics likely decrease the number of daily urge incontinence episodes.»B | Kuiva suu 18 %, ummetus 3 %, vatsakipu 2 %, virtsaretentio 1 %, kuivat silmät 1 % | Haitat korostuvat erityisesti iäkkäillä (ks. Iäkkäiden virtsankarkailun diagnostiikka ja hoito «A4»6). |
| Paikallisestrogeeni | Saattaa vähentää, ks. tarkemmin näytönastekatsaus «Topical estrogen therapy may reduce urinary incontinence symptoms.»C | Vähäiset haitat | |
| Prasteroni | - | - | Prasteronista ei ole vielä luotettavaa tutkimusnäyttöä. |
| Säärihermostimulaatio | - | Vähäiset haitat | Todennäköisesti vähentää hieman kokonaisoireita «Percutaneous Tibial nerve stimulation (PTNS) likely decreases overactive bladder symptoms slightly.»B. |
| Rakkokoulutus | Tutkimusnäyttö vaikutuksista epävarmaa «The evidence on bladder training to treat incontinence symptoms is very uncertain.»D | Vähäiset haitat | |
| Laihdutus | -26 % (-0,57 kertaa) «Weight loss likely decreases urinary incontinence episodes.»B | Vähäiset haitat | Vaikutusarvio perustuu tutkimukseen, jossa painonpudotusohjelma vähensi painoa 6,3 kg vertailuryhmään nähden. |
| Erikoissairaanhoito | |||
| Botuliinitoksiinipistos | -43 % (-1,9 kertaa) «Onabotulinum-toxin A decreases urinary incontinence episodes.»A | Virtsaumpi 1,9 %, kipu virtsatessa 2,5 % | Tutkimuksiin osallistuneiden potilaiden oireet olivat keskimäärin vaikeat. Tämä selittää virtsankarkailukertojen suuren absoluuttisen vähenemisen. |
- Suomessa ovat saatavilla
- antikolinergiset lääkkeet darifenasiini, fesoterodiini, oksibutyniini, solifenasiini, tolterodiini ja trospiumkloridi
- beeta3-agonistit mirabegroni ja vibegroni.
- Eri valmisteiden välillä ei liene merkittävää eroa hoidon hyödyn suhteen «Herbison P, McKenzie JE. Which anticholinergic is ...»99, «Zhang J, Chi J, Lou K, ym. Comparison of efficacy ...»100.
- Valmisteiden haitat kuitenkin vaihtelevat (ks. taulukko «Pakkovirtsankarkailun hoitovaihtoehdot ja virtsankarkailukertojen määrä 8–12 viikon
seurannassa....»2).
- Mirabegroni ei todennäköisesti aiheuta merkittävää verenpaineen nousua. Takykardia sen sijaan saattaa olla mahdollinen harvinainen haitta (alle 1 % potilaista) «Chapple CR, Cruz F, Cardozo L, ym. Safety and Effi...»101.
- Jos pakkovirtsankarkailun syy on neurologinen sairaus, kuten selkäydinvamma, virtsarakko voi kehittyä korkeapaineiseksi, mikä altistaa munuaisvauriolle. Antikolinergit vähentävät rakkopainetta «Madersbacher H, Mürtz G, Stöhrer M. Neurogenic det...»102 ja saattavat olla usein parempi valinta neurologisen sairauden aiheuttamaan virtsankarkailuun.
- Vasta-aiheet:
- Antikolinergien käytön vasta-aiheita ovat virtsaumpi, hallitsematon ahdaskulmaglaukooma, myasthenia gravis ja vaikea paksusuolitulehdus. Ks. myös tarvittaessa kappale Iäkkäiden diagnostiikka ja hoito «A00:00:00.388066000»10.
- Beeta3-agonistien käytön vasta-aiheita ovat loppuvaiheen munuaissairaus, vaikea maksan vajaatoiminta, vakava ja hallitsematon hypertensio tai pidentynyt QT-aika «Zhang J, Chi J, Lou K, ym. Comparison of efficacy ...»100, «Chapple CR, Cruz F, Cardozo L, ym. Safety and Effi...»101.
Erikoissairaanhoidossa toteutettava hoito
Virtsarakon botuliinitoksiinihoito
- Botuliinitoksiini A:n ruiskutus rakkolihakseen vähentää virtsankarkailukertojen määrää
«Onabotulinum-toxin A decreases urinary incontinence episodes.»A. Se on ilmeisesti muita lääkehoitoja tehokkaampi pakkovirtsakarkailun hoidossa «Drake MJ, Nitti VW, Ginsberg DA, ym. Comparative a...»105.
- Tässä uusimista edellyttävässä hoitomuodossa yhden hoitokerran vaikutus kestää noin 6 kuukautta. Ks. lisätietoaineisto «Botuliinitoksiinin ruiskutus virtsarakkolihakseen pakkovirtsankarkailun hoidossa»14 ja kuva «Kuva botuliinin ruiskutuksesta virtsarakon seinämään»4.
- Virtsaumpi kehittyy noin 2 %:lle potilaista. Noin 2 % potilaista kokee toimenpiteen jälkeen kipua virtsatessa.
- Hoidon vasta-aiheet ovat yliherkkyys botuliinitoksiini A:lle tai liuoksen apuaineille, virtsatieinfektio hoitoajankohtana, virtsaumpi, jota potilas ei katetroi säännöllisesti, tai kyvyttömyys tai haluttomuus aloittaa hoidon jälkeinen katetrointi, jos siihen syntyy tarvetta, ks. lääkeinfo.fi «https://laakeinfo.fi/documents/7350»3.
Kirurginen hoito pakkovirtsankarkailussa
- Jos pakkovirtsankarkailun hoidossa konservatiivisilla tai vähän kajoavilla menetelmillä
(lääkehoidot, fysioterapia, botuliinitoksiini A:n ruiskutus rakkolihakseen) ei saavuteta
tyydyttävää virtsanpidätyskykyä, voidaan erikoissairaanhoidossa harkita sakraalisen
neuromodulaattorin laittoa tai viimeisenä vaihtoehtona rakon muovaamista matalapaineiseksi
suolipaikkaa käyttämällä (simpukkakystoplasia) tai virtsa-avannetta.
- Sakraalisen neuromodulaation vaikutus pakkovirtsankarkailuun lienee samaa luokkaa kuin rakkolihakseen ruiskutettavien botuliinitoksiini A -pistoksien «Amundsen CL, Richter HE, Menefee SA, ym. Onabotuli...»103, «Amundsen CL, Komesu YM, Chermansky C, ym. Two-Year...»104. Laite jouduttiin satunnaistetussa tutkimuksessa poistamaan komplikaation vuoksi 4 %:lta potilaista.
- Simpukkakystoplastiapotilailla on usein neurogeeninen rakkohäiriö tai jostain muusta syystä kutistunut rakko. Toimenpiteen jälkeen rakko on tyhjennettävä toistokatetroimalla «Campbell JD, Gries KS, Watanabe JH, ym. Treatment ...»106, «Edlund C, Peeker R, Fall M. Clam ileocystoplasty: ...»107.
- Virtsa-avanneleikkaus on syytä tehdä etenkin silloin, jos neurogeenisen pakkovirtsankarkailun lisäksi korkeapaineinen rakko uhkaa vaurioittaa munuaisia eikä simpukkakystoplastia ole jostain syystä mahdollinen «Luangkhot R, Peng BC, Blaivas JG. Ileocecocystopla...»108, «Robertson AS, Davies JB, Webb RJ, ym. Bladder augm...»109.
- Pakkovirtsankarkailun leikkaushoidosta vastaavat urologit.

Kuva botuliinin ruiskutuksesta virtsarakon seinämään.
Kuvan lähde: Vaarala M, Perttilä I, Hellström P. Botuliini auttaa myös urologisissa ongelmissa. Duodecim 2010;126:2511-7
Ponnistusvirtsankarkailun hoito
Suositus: Suosittele ponnistusvirtsankarkailun ensilinjan hoidoksi lantionpohjan lihasharjoittelua.
- Lantionpohjan ohjeistetulla lihasharjoittelulla on todennäköisesti suuri vaikutus virtsankarkailun määrään «Pelvic floor muscle exercise likely decreases the urinary incontinence symptoms.»B. Oireet vähenivät keskimäärin noin 50 %.
- Harkitse potilaan ohjaamista lantionpohjan fysioterapiaan, jos potilas ei osaa supistaa lantionpohjan lihaksia (sormitesti) «Lantionpohjan lihasten sormitestaus»6, «Lantionpohjan lihasten harjoitteluohje»9.
- Ohjaa potilas erikoissairaanhoitoon, jos ponnistusvirtsankarkailun oireet ovat vaikeat «Labrie J, Berghmans BL, Fischer K, ym. Surgery ver...»110 tai säännöllinen lantionpohjan lihasharjoittelu ei tuota riittävää apua.
Emättimeen asetettava virtsaputken tuki
- Emättimeen asetettava tuki saattaa helpottaa ponnistusvirtsankarkailun oireita, mutta tutkimusnäyttö on hyvin epävarmaa «A vaginal support device may decrease stress urinary incontinence symptoms, but the evidence is very uncertain.»D.
- Tuki voi olla hyvä vaihtoehto potilaille, joilla ponnistusvirtsankarkailua esiintyy vain tietyissä tilanteissa, kuten raskaissa liikuntaharrastuksissa.
- Haitat lienevät kuitenkin vähäisiä.
- Katso tarkemmin lisätietoaineistosta «Emättimeen asetettava tuki ponnistusvirtsankarkailun hoidossa»15.
Lääkehoito
- Lääkkeiden merkitys ponnistuskarkailun hoidossa on vähäinen.
- Duloksetiini todennäköisesti vähentää virtsankarkailukertojen määrää hieman «Duloxetine likely decreases incontinence episodes slightly in patients with stress urinary incontinence.»B.
- Haittavaikutustensa (erityisesti pahoinvoinnin) takia duloksetiinin käyttö on vähäistä (ks. alla oleva taulukko «Ponnistusvirtsankarkailun hoitovaihtoehdot ja virtsankarkailukertojen määrä 8–12 viikon seurannassa....»3).
| Hoito | Virtsankarkailukertojen väheneminen (per 24 t) [näytönaste] | Yleiset haitat – lääkkeen vuoksi haitan saavien potilaiden osuus (riskiero)*** | Kommentit | |
|---|---|---|---|---|
| * Hyöty kuvaa suhteellista virtsankarkailun vähenemää. Keskimääräinen absoluuttinen
hoitovaikutus vaihtelee potilaan lähtötason ja oireiden luonnollisen kulun mukaan.
Myös lääkkeen hoitovaikutuksessa saattaa olla yksilöllisiä eroja. ** Esimerkiksi jos potilaan virtsankarkailu vähenee seurannassa 20 % ilman hoitoa, beeta3-agonistilääkitys huomioiden virtsankarkailu vähentyisi 42 %. Virtsankarkailun väheneminen seurannassa = Lähtötaso – kipu seurannassa ilman hoitoa x hoitovaikutus = 1 – 0,8 x 0,72 = 0,42. *** Riskiero (risk difference) lumeeseen / hoitamatta jättämiseen verrattuna. Todellisuudessa haittaa saa useampi, koska moni saa usein haittatapahtuman myös ilman hoitoa ja kyseinen oire saattaa lääkkeen vuoksi pahentua. Taulukoita varten arvioimme hoitojen suhteellista hyötyä verrattuna hoitamatta jättämiseen. Menetelmät on kuvattu lisätietomateriaalissa «Calculation of relative mean difference»13. |
||||
| Oireiden luonnollinen kulku vaihtelee huomattavasti yksilöiden välillä, ja lääkevaikutuksissakin saattaa olla yksilöllisiä eroja. Keskimäärin oireet vähenevät seurannassa myös ilman hoitoa, minkä vuoksi lääkevaikutuksen erottaminen oireiden luonnollisesta kulusta voi olla vaikeaa. | ||||
| Lantiopohjan lihasharjoittelu | -54 % (-1,23 kertaa) «Pelvic floor muscle exercise likely decreases the urinary incontinence symptoms.»B | Vähäiset haitat | ||
| Duloksetiini | -23 % (-0,41 kertaa) «Duloxetine likely decreases incontinence episodes slightly in patients with stress urinary incontinence.»B | Ei suoraa näyttöä haitoista. Depression hoidossa: pahoinvointi 16 %, kuiva suu 8 %, uneliaisuus 6 %, huimaus 5 %, ummetus 4 %, hikoilu 4 % |
||
| Laihdutus | -26 % (-0,57 kertaa) «Weight loss likely decreases urinary incontinence episodes.»B | Vähäiset haitat | Vaikutusarvio perustuu tutkimukseen, jossa painonpudotusohjelma vähensi painoa 6,3 kg vertailuryhmään nähden. | |
| Erikoissairaanhoito | ||||
| Polyakryyliamidihydrogeeli | Vähäinen tutkimusnäyttö. Nauhaleikkaukseen nähden hyöty todennäköisesti vähäisempi. | Ohimenevä virtsaumpi 3–6 %, ohimenevä kipu pistoskohdassa 12 % «Itkonen Freitas AM, Mentula M, Rahkola-Soisalo P, ...»111, «Sokol ER, Karram MM, Dmochowski R. Efficacy and sa...»112 |
Viiden vuoden seurannassa kolmannes potilaista tarvitsee kaksi injektiohoitoa ja kolmannes päätyy nauhaleikkaukseen (uusiutuva virtsankarkailu). | |
| Nauhaleikkaus | Vähentää todennäköisesti huomattavasti oireita suhteessa fysioterapiaan «Leikkaushoito todennäköisesti vähentää virtsankarkailun oireita suhteessa fysioterapiaan keskivaikean ja vaikean ponnistusvirtsankarkailun hoidossa.»B | Retropubinen vs transobturatorinen leikkaus: uusintaleikkaus (1 vs 11 %) virtsaamisvaikeus (7 vs 4 %) nivuskipu (1 vs 6 %) alavatsakipu (3 vs 1 %) uusiutuva virtsankarkailu (8,2 % vs 8,5 %) |
Yli 80 % potilaista kokee virtsankarkailuoireiden väistyvän kokonaan leikkauksen jälkeen (vuoden seuranta). | |
| Ei vaikutusta virtsankarkailuun tai vaikutus kliinisesti merkityksetön | ||||
| Laserhoito | Vaikutus todennäköisesti merkityksetön tai vaikutusta ei ole «Vaginal laser therapy provides little or no benefit on stress urinary incontinence symptoms.»B | Vakavat haitat harvinaisia. Tarkempi arvio haitoista puuttuu. | Tutkimuksiin osallistuneet potilaat olivat enimmäkseen sellaisia, joilla oli konservatiivisesta hoidosta huolimatta haittaavat oireet. | |
Ponnistusvirtsankarkailun hoito erikoissairaanhoidossa
Täyteaineet
- Polyakrylamidihydrogeeli on yleisin virtsaputken ympärille ruiskutettava täyteaine «Virtsaputken ympärille ruiskutettavan polyakrylamidihydrogeelin ruiskutustekniikka ja ruiskutuskohdat»5, jota käytetään ponnistusinkontinenssin hoitoon. Menetelmä soveltuu erityisesti potilaille, jotka toivovat vähän kajoavaa hoitoa, joiden leikkausriski on suurentunut tai joille tehty leikkaushoito ei ole ollut tehokas.
- Hoito on turvallinen, ja komplikaatiot ovat harvinaisia «Itkonen Freitas AM, Mentula M, Rahkola-Soisalo P, ...»111, «Lamblin G, Boix S, Moret S, ym. Effectiveness and ...»113 (ks. taulukko «Ponnistusvirtsankarkailun hoitovaihtoehdot ja virtsankarkailukertojen määrä 8–12 viikon seurannassa....»3 yllä).
- Hoidon vaikuttavuudesta suhteessa konservatiivisiin hoitoihin (lääkehoito tai lihasharjoittelu) ei ole tutkimusnäyttöä.
- Nauhaleikkaushoito todennäköisesti vähentää virtsankarkailua täyteaineinjektiota enemmän. Satunnaistetussa tutkimuksessa vuoden jälkeen hoidosta 84 % leikkauspotilaista ja 23 % täyteaineella hoidetuista koki oireiden väistyneen «Itkonen Freitas AM, Mentula M, Rahkola-Soisalo P, ...»111. Viiden vuoden päästä luvut olivat 62 % ja 36 % «Freitas AI, Isaksson C, Rahkola-Soisalo P, ym. Ten...»114.
- Hoidon toistaminen on melko yleistä. Uusintatoimenpide – joko uusi injektio tai nauhaleikkaus – tehdään 27–70 %:lle potilaista viiden vuoden aikana «Svenningsen R, Oversand SH, Schiøtz HA, ym. Compar...»115, «Itkonen Freitas AM, Mentula M, Rahkola-Soisalo P, ...»111.
Nauhaleikkaus
- Nauhaleikkauksessa asetetaan sulamaton polypropyleeninauha virtsaputken keskiosan alle (kuvat «Mini-invasiiviset toimenpiteet ponnistusvirtsankarkailun leikkaushoidossa, kuva 1»6 ja «Mini-invasiiviset toimenpiteet ponnistusvirtsankarkailun leikkaushoidossa, kuva 2»7), «Ulmsten U, Falconer C, Johnson P, ym. A multicente...»116.
- Nauhaleikkaushoito todennäköisesti vähentää virtsankarkailun määrää fysioterapiaa enemmän keskivaikean ja vaikean virtsankarkailun hoidossa «Leikkaushoito todennäköisesti vähentää virtsankarkailun oireita suhteessa fysioterapiaan keskivaikean ja vaikean ponnistusvirtsankarkailun hoidossa.»B.
- Suomalaisessa aineistossa ponnistusvirtsankarkailulle diagnostinen yskäisytesti oli
negatiivinen 95 %:lla nauhaleikkauksella hoidetuista ja 82 %:lla täyteaineryhmässä «Freitas AI, Isaksson C, Rahkola-Soisalo P, ym. Ten...»114.
- Potilaista 66 %:lla sekä vaippatesti että yskäisytesti olivat negatiivisia (vrt. 48 %:lla täyteaineryhmässä) .
- Potilaista 62 % koki itsensä oireettomaksi viiden vuoden kuluttua hoidosta «Freitas AI, Isaksson C, Rahkola-Soisalo P, ym. Ten...»114.
- Retropubiset (TVT) ja transobturatoriset (TOT/TVT-O) leikkaukset ovat todennäköisesti lyhyessä seurannassa yhtä tehokkaita, mutta uusintaleikkausten riski on suurempi transobturatorisen leikkauksen jälkeen «Transobturator and retropubic slings are likely as effective in decreasing incontinence symptoms.»B.
- Leikkauksen haitat vaihtelevat hieman leikkaustekniikan mukaan (ks. taulukko «Ponnistusvirtsankarkailun hoitovaihtoehdot ja virtsankarkailukertojen määrä 8–12 viikon seurannassa....»3 yllä).
- Leikkauksen voi tehdä paikallispuudutuksessa.
- Urodynaaminen tutkimus ei paranna hoitotuloksia, kun on kyse primaarisesta (myös kliinisessä tutkimuksessa todetusta) ponnistusvirtsankarkailusta «Clement KD, Lapitan MC, Omar MI, ym. Urodynamic st...»117.
- Leikkaukselle ei ole ehdottomia vasta-aiheita. Suhteellisia vasta-aiheita ovat virtsaamisvaikeus sekä anatomiset poikkeavuudet, vaikeat asentorajoitteet ja merkittävä lihavuus (BMI > 35), jolloin toimenpide voi olla teknisesti haastava.
- Nauhaleikkauksen «Zyczynski HM, Albo ME, Goldman HB, ym. Change in O...»118, «Jha S, Jeppson PC, Dokmeci F, ym. Management of mi...»119 hoitotulos lienee heikompi sekamuotoisen virtsankarkailun hoidossa kuin pelkän ponnistusvirtsankarkailun hoidossa «Richter HE, Diokno A, Kenton K, ym. Predictors of ...»120.
- Synnytys (alatiesynnytys tai keisarileikkaus) nauhaleikkauksen jälkeen ei lisää virtsankarkailun uusimisen tai uusintatoimenpiteen riskiä «Ruffolo AF, Lallemant M, Garabedian C, ym. The imp...»121.
- Mininauhaleikkauksia tulee toistaiseksi pitää kokeellisina.
Nauhaleikkauksen yhdistäminen laskeumaleikkauksiin
- Laskeumaan voi liittyä virtsankarkailua tai tihentynyttä virtsaamistarvetta, jotka saattavat helpottua laskeuman korjauksella.
- Noin 10–20 %:lle saattaa laskeumaleikkauksen seurauksena ilmaantua virtsankarkailua «Maher C, Feiner B, Baessler K, ym. Surgical manage...»122, «Khayyami Y, Elmelund M, Lose G, ym. De novo urinar...»123.
- Tavallisimmin tehdään ensin laskeumaleikkaus ja tarvittaessa myöhemmin nauhaleikkaus.
- Noin kolmasosa potilaista saa pelkästä laskeumaleikkauksesta riittävän avun virtsankarkailuun, joten laskeumaleikkauksen ja nauhaleikkauksen yhdistäminen altistaa nämä potilaat turhalle nauhaleikkaukselle «Borstad E, Abdelnoor M, Staff AC, ym. Surgical str...»124, «Lensen EJ, Withagen MI, Kluivers KB, ym. Urinary i...»125.
Muut leikkaukset ja kajoavat hoidot
- Muita leikkaushoitoja ja kajoavia hoitoja on käsitelty lisätietomateriaalissa «Muut leikkaukset ja kajoavat hoidot»16.
Uusiutuneen ponnistusvirtsankarkailun kajoava hoito
- Kajoavan hoidon epäonnistumiselle altistavat aiemmat tehdyt muut inkontinenssileikkaukset, suuri karkaavan virtsan määrä, sekamuotoinen virtsankarkailu, vaikea ylipaino ja matalapaineinen virtsaputki (ISD) «Richter HE, Litman HJ, Lukacz ES, ym. Demographic ...»126, «Hellberg D, Holmgren C, Lanner L, ym. The very obe...»127, «Nager CW, Sirls L, Litman HJ, ym. Baseline urodyna...»128, «Braga A, Caccia G, Papadia A, ym. Urethral bulking...»129.
- Aiemman nauhaleikkauksen tai täyteaineen ruiskutuksen jälkeen uusiutuneen ponnistusvirtsankarkailun
hoitoon voidaan harkita uutta nauhaleikkausta tai täyteaineen ruiskutusta, mutta uusintahoitojen
tuloksista ei ole juuri tutkimusnäyttöä «Bakali E, Buckley BS, Hilton P, ym. Treatment of r...»130 ja hoito perustuu pitkälti kliiniseen kokemukseen.
- Uusintanauhaleikkausten tulokset voivat olla huonommat kuin ensileikkausten «Ruffolo AF, Melocchi T, Frigerio M, ym. Efficacy a...»131.
- Nauhaleikkauksen jälkeen uusiutuneen ponnistusvirtsankarkailun ruiskutushoidosta saa hyötyä 64–85 % potilaista «Braga A, Caccia G, Papadia A, ym. Urethral bulking...»129.
- Jäännösvirtsan mittaus kuuluu uusiutuneen virtsankarkailun perustutkimuksiin.
- Urodynaamiset mittaukset ja nauhan tai täyteaineen sijainnin määrittäminen ultraäänellä ennen uusintaleikkausta voivat auttaa hoidon suunnittelussa.
- Aiempien leikkausten jäljiltä liikkumaton, fiksoitu virtsaputki heikentää uuden nauhaleikkauksen tuloksia «Lo TS, Horng SG, Chang CL, ym. Tension-free vagina...»132, «Liapis A, Bakas P, Lazaris D, ym. Tension-free vag...»133, «Goldman HB, Rackley RR, Appell RA. The efficacy of...»134.
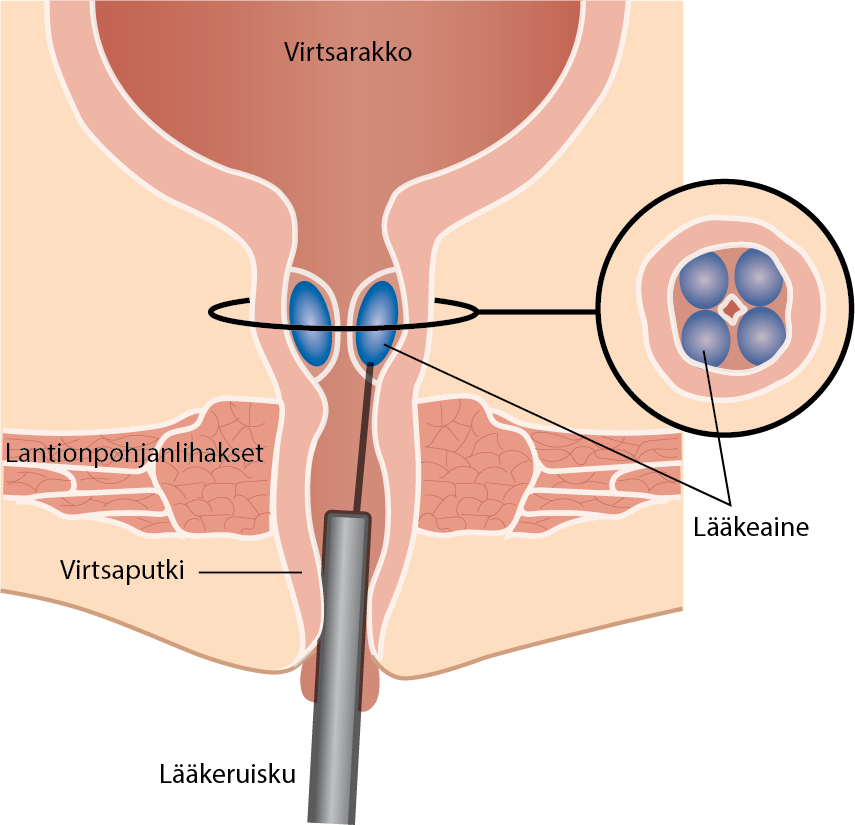
Virtsaputken ympärille ruiskutettavan polyakrylamidihydrogeelin ruiskutustekniikka ja ruiskutuskohdat.
© Suomalainen Lääkäriseura Duodecim

Mini-invasiiviset toimenpiteet ponnistusvirtsankarkailun leikkaushoidossa, kuva 1.
Kaavakuva retropubisen nauhan sijainnista.
© Suomalainen Lääkäriseura Duodecim

Mini-invasiiviset toimenpiteet ponnistusvirtsankarkailun leikkaushoidossa, kuva 2.
Kaavakuva transobturatorisesen nauhan sijainnista.
© Suomalainen Lääkäriseura Duodecim
Iäkkäiden virtsankarkailun diagnostiikka ja hoito
Suositus: Suosi lääkkeettömiä hoitoja iäkkäiden virtsankarkailun hoidossa.
- Iäkkäille soveltuvat samat lääkkeettömät hoidot kuin muillekin virtsankarkailusta kärsiville.
- Fyysinen aktiivisuus ja liikunta- ja toimintakyvyn ylläpito saattavat ehkäistä virtsankarkailua «Danforth KN, Shah AD, Townsend MK, ym. Physical ac...»135, «Kim MM, Ladi-Seyedian SS, Ginsberg DA, ym. The Ass...»40, mikä on hyvä huomioida myös kuntouttavassa hoitotyössä.
Suositus: Älä ilman erityisiä perusteita määrää iäkkään virtsankarkailun hoitoon antikolinergisia lääkkeitä.
- Haitat ylittävät useimmiten hyödyt. Beeta3-agonistihoidon haitat ovat vähäisemmät kuin antikolinergihoidon (taulukko «Pakkovirtsankarkailun hoitovaihtoehdot ja virtsankarkailukertojen määrä 8–12 viikon seurannassa....»2).
- Virtsankarkailusta tulee keskustella kaikenikäisten naisten kanssa «Visser E, de Bock GH, Messelink EJ, ym. Active enc...»136.
- Ikä sinällään ei rajaa diagnostiikkaa tai hoitovaihtoehtoja, mutta toimintakyky, gerastenia, kognitio ja muut sairaudet tulee huomioida hoitoa valittaessa.
- Iäkkään monisairaan potilaan hoidosta kannattaa konsultoida geriatria.
Diagnostiikka
- Lähestymistavan tulee olla kokonaisvaltainen, sillä iäkkäiden virtsankarkailu on usein
monitekijäinen.
- Selvittelyyn kuuluvat muun muassa elintavat, perussairauksien hoitotasapaino, kokonaislääkitys, kognitio, mieliala, ravitsemustila, suolen toiminta (ummetus), suoriutuminen päivittäistoiminnoista ja liikuntakyky apuvälineineen.
- Virtsankarkailu on yhteydessä kaatumisiin, joten myös muut kaatumisten riskitekijät on hyvä huomioida «Moon S, Chung HS, Kim YJ, ym. The impact of urinar...»137.
- Tarvittaessa voi hyödyntää esimerkiksi kotihoidon palvelutarpeen kartoituksessa tehtyä toimintakykyarviota, kliinistä gerastenia-asteikkoa «Clinical Frailty Scale»8 tai molempia.
- On hyvä muistaa ylivuotovirtsankarkailun mahdollisuus ja tarkistaa tarvittaessa jäännösvirtsan määrä «Gibson W, Johnson T, Kirschner-Hermanns R, ym. Inc...»138.
- Erityisesti on huomioitava ummetus ja virtsarakon toimintaan vaikuttavat lääkkeet (ks. taulukko «Virtsankarkailua mahdollisesti aiheuttavia tai pahentavia lääkeaineita, jotka on syytä huomioida erityisesti iäkkäiden hoidossa....»4) ja mahdolliset laskeumat.

Clinical Frailty Scale.
© 2005–2020 Rockwood, Version 2.0 (FI)
Kuvan lähde: Rockwood K ym. A global clinical measure of fitness and frailty in elderly people. CMAJ 2005:173;489-495
Iäkkäiden hoidon erityispiirteet
- Kokonaisvaltainen geriatrinen arvio auttaa jäsentämään kokonaishoitoa ja tukee yksilöllistä hoidon suunnittelua. Ks. Käypä hoito -suositus Monisairas potilas «Monisairas potilas»7, «Monisairas potilas. Käypä hoito -suositus. Suomala...»139.
- Arviossa on hyvä huomioida potilaan odotukset hoidon suhteen.
- Lääkkeettömät hoidot ovat ensisijaisia.
- Hoidon tavoitteena on mahdollisimman hyvä toimintakyky ja elämänlaatu.
Elintapamuutokset
- Juomisen rajoittamista lienee syytä välttää kuivumisvaaran vuoksi.
- Ummetusta on tärkeää ehkäistä ja hoitaa.
- Laihdutus ei ole iäkkäiden virtsankarkailun ensisijainen hoito, koska se voi johtaa
lihasvoimien- ja massan vähenemiseen (sarkopenia).
- Iäkkäiden BMI:n normaalipainon viiterajat ovat korkeammat kuin nuorempien aikuispotilaiden «Suominen MH, Jyvakorpi SK, Pitkala KH, ym. Nutriti...»140.
- Tavoitteena tulisi olla riittävän monipuolinen ravitsemus ja liiallisen laihtumisen estäminen.
Fyysinen harjoittelu ja käyttäytymiseen perustuvat hoitomuodot
- Lantionpohjan lihasten ohjattu harjoittelu erikseen tai yhdistettynä lihaskuntoharjoitteluun
saattaa vähentää itsenäisesti ja kotihoidon tuella asuvien iäkkäiden naisten virtsankarkailua
«Kim H, Yoshida H, Suzuki T. The effects of multidi...»141, «Kim H, Suzuki T, Yoshida Y, ym. Effectiveness of m...»142, «Engberg S, Sereika SM. Effectiveness of Pelvic Flo...»143, «Talley KMC, Wyman JF, Bronas U, ym. Defeating Urin...»144.
- Lievä kognition heikentyminen ei ole este harjoittelulle.
- Tuetusti tai ympärivuorokautisessa hoidossa asuvat saattavat hyötyä käyttäytymiseen perustuvista hoitomuodoista, kuten aikataulutetusta WC:ssä käyttämisestä ja virtsaamiskehotusohjelmasta.
- Virtsankarkailu on yleistä pitkälle edennyttä muistisairautta sairastavilla «Virtsankarkailun esiintyvyys neurologisissa sairauksissa»1.
- WC:hen avustaminen osana kuntouttavaa hoitotyötä edistää kuivana pysymistä.
Lääkehoito
- Paikallinen estrogeeni soveltuu hyvin myös iäkkäiden pakkovirtsankarkailuoireiden hoitoon.
- Ennen virtsankarkailun lääkehoidon aloitusta tulisi lääkehoidon kokonaisarvioinnissa huomioida rakon tyhjenemiseen vaikuttavat ja virtsankarkailua pahentavat lääkkeet (ks. taulukko «Virtsankarkailua mahdollisesti aiheuttavia tai pahentavia lääkeaineita, jotka on syytä huomioida erityisesti iäkkäiden hoidossa....»4).
- Antikolinergien haittavaikutukset ylittävät useimmiten mahdolliset hyödyt «Kay GG, Granville LJ. Antimuscarinic agents: impli...»145, «Kraus SR, Bavendam T, Brake T, ym. Vulnerable elde...»146.
- Antikolinergisen lääkkeen aloitusta on syytä välttää erityisesti, mikäli potilaalla on jo muita antikolinergisesti vaikuttavia lääkkeitä.
- Vakavimpia haittoja ovat virtsaumpi, kognitiiviset häiriöt ja sekavuus «Samuelsson E, Odeberg J, Stenzelius K, ym. Effect ...»147, «Stoniute A, Madhuvrata P, Still M, ym. Oral antich...»148.
- Antikolinergit saattavat lisätä myös kaatumisen ja luunmurtuman riskiä «Reinold J, Schäfer W, Christianson L, ym. Antichol...»149.
- Ks. myös Vältä viisaasti -suositus «Antikolinergit iäkkäiden potilaiden virtsaamisoireiden hoidossa»17.
- Antikolinergit ja Alzheimerin taudin hoitoon käytettävät asetyylikoliiniesteraasin estäjät (AKE:n estäjät) heikentävät toistensa tehoa, joten niiden yhteiskäyttöä lienee syytä välttää. Ks. Käypä hoito -suositus Muistisairaudet «Muistisairaudet»8 «Muistisairaudet. Käypä hoito -suositus. Suomalaise...»150.
- Beeta3-agonisti saattaa vähäisempien haittojen vuoksi olla antikolinergeja parempi
vaihtoehto iäkkäille.
- Alle 1 % potilaista voi saada lääkkeestä sydämentykytystä «Chapple CR, Cruz F, Cardozo L, ym. Safety and Effi...»101.
- Pienempi lääkehoidon aloitusannos saattaa vähentää haittoja.
- Tehoton lääkehoito tulee lopettaa.
Muut hoidot
- Hauraiden ja monisairaiden hoidossa on syytä huomioida toimenpiteisiin liittyvien komplikaatioiden ja haittojen riski «Parker-Autry CY, Bauer S, Ford C, ym. Examining th...»151.
- Botuliinitoksiini-injektiot soveltuvat myös iäkkäiden vaikean pakkovirtsankarkailun hoitoon «Kao YL, Ou YC, Kuo HC. Bladder Dysfunction in Olde...»152.
- Nauhaleikkaus vähentänee myös iäkkäiden ponnistusvirtsankarkailua. Hyödyt saattavat olla kuitenkin vähäisemmät kuin nuoremmilla potilailla «Malek JM, Ellington DR, Jauk V, ym. The effect of ...»153.
- Iäkkäiden hoidossa kannattaa harkita täyteaineita niiden nauhaleikkausta vähäisempien haittojen vuoksi «Faurie B, Hascoet J, Richard C, ym. Outpatient Per...»154.
- Ihon pinnalta toteutettava säärihermon sähköstimulaatio soveltunee myös iäkkäiden pakkovirtsankarkailun hoitoon «Schreiner L, Nygaard CC, Dos Santos TG, ym. Transc...»155, «Schreiner L, dos Santos TG, Knorst MR, ym. Randomi...»156.
Vältä viisaasti -suositus: Älä hoida iäkkäiden oireetonta bakteriuriaa, sillä se ei vähennä kastelua, myöhempiä virtsatieinfektioita eikä kuolleisuutta «Oireettoman bakteriurian hoito iäkkäillä»18.
- Mikäli oireet viittaavat virtsatietulehdukseen (esimerkiksi äkillinen alku tai paheneminen, muut virtsatietulehduksen oireet ja löydökset), harkitse antibioottihoitoa.
Ylivuotovirtsankarkailu
- Iäkkäidenkin ylivuotovirtsankarkailun hoidoksi soveltuu parhaiten toistokatetrointi, jotta vältetään kestokatetroinnin aiheuttamat haitat.
- Ummetus ja rakkoa lamaavat lääkeaineet on syytä huomioida (ks. taulukko «Virtsankarkailua mahdollisesti aiheuttavia tai pahentavia lääkeaineita, jotka on syytä huomioida erityisesti iäkkäiden hoidossa....»4).
| Lääkeaine | Vaikutustapa |
|---|---|
| Alfa-adrenergiset antagonistit (esim. tamsulosiini ja alfutsosiini) | Vähentävät sileän lihaksen tonusta virtsaputkessa, ponnistusvirtsankarkailu |
| Angiotensiinikonvertaasin (ACE:n) estäjät | Yskä, ponnistusvirtsankarkailu |
| Antihistamiinit | Sekavuus |
| Antikolinergit | Tyhjenemisvaikeudet, virtsaumpi, ummetus, ylivuotovirtsankarkailu, kognitiiviset häiriöt, WC:ssä käyntitaitojen heikentyminen |
| Asetyylikolinesteraasin (AKE:n) estäjät (Alzheimerin taudissa käytettävät) | Virtsarakon supistumisherkkyyden lisääntyminen, pakkovirtsankarkailu |
| Bentsodiatsepiinit | Sekavuus, liikuntakyvyn heikentyminen |
| Diureetit | Virtsanerityksen ja virtsamäärän lisääntyminen, pakkovirtsankarkailu |
| Gabapentiini | Turvotus, yöllinen polyuria, sekavuus |
| Kalsiuminestäjät | Tyhjenemisvaikeudet, virtsaumpi, ummetus |
| Litium | Polyuria |
| Opiaatit | Tyhjenemisvaikeudet, virtsaumpi, ummetus, sekavuus, liikuntakyvyn heikentyminen |
| Psykoosilääkkeet | Antikolinergivaikutukset |
| Serotoniinin takaisinoton estäjät (SSRI-lääkkeet) | Kolinerginen, rakkosupistuksia lisäävä vaikutus |
| Tulehduskipulääkkeet | Turvotus, yöllinen polyuria |
Apuvälineet ja hoitotarvikkeet
- Virtsankarkailun hoidon apuvälineisiin ja hoitotarvikkeisiin kuuluvat imukykyiset
siteet, vuotosuojat, vuoteensuojat, emättimeen asetettavat tuet «Emättimeen asetettava tuki ponnistusvirtsankarkailun hoidossa»15 ja virtsakatetrit.
- Aiheeseen perehtyneen terveydenhuollon ammattilaisen ohjauksella oikein valittu apuväline parantaa potilaan elämänlaatua ja vähentää apuvälineistä syntyviä kustannuksia «Nuotio M, Ala-Nissilä S, Tammela T. Iäkkäiden virt...»157, «Cilluffo S, Terzoni S, Destrebecq A, ym. Efficacy,...»158.
- Jos apuvälineenä käytetään siteitä tai vuotosuojia, terveydenhuollon ammattilaisen tulee iho-ongelmien synnyn ehkäisemiseksi arvioida ja tehdä potilaskohtainen suunnitelma oikeasta tuotteesta, määrästä ja vaihtovälistä «Banharak S, Panpanit L, Subindee S, ym. Prevention...»159, «Sosiaali- ja terveysministeriö. Valtakunnalliset l...»160.
- Ponnistusvirtsankarkailun hoitoon voidaan käyttää erilaisia emättimeen asetettavia tukia, kuten renkaita, tamponeja tai pessaareita, mutta näiden vaikuttavuudesta tai keskinäisestä paremmuudesta ei ole selvää näyttöä «A vaginal support device may decrease stress urinary incontinence symptoms, but the evidence is very uncertain.»D.
- Jos potilaan liikkumis- ja toimintakyky on rajoittunut, WC:ssä käymistä tulee helpottaa
vaatetuksen, liikkumisapuvälineiden ja kodin muutostöiden avulla «Gibson W, Johnson T, Kirschner-Hermanns R, ym. Inc...»138, «Sosiaali- ja terveysministeriö. Valtakunnalliset l...»160.
- Vaatteiden tulee olla helposti avattavia ja riisuttavia.
- WC-istuinkorotus helpottaa niveloireisen virtsaamista.
- Liikuntarajoitteiset voivat vaippojen sijasta käyttää siirrettävää WC-istuinta, naisille suunniteltua virtsapulloa tai alusastiaa.
- Kotona tehtäviä muutoksia WC:ssä käynnin helpottamiseksi ovat kodin riittävä valaistus, kiinteät tukikaiteet sekä liikkumista hidastavien mattojen ja kynnysten poisto. Oman hyvinvointialueen fysio- tai toimintaterapeutti tekee liikkumisen ja kodin muutostöiden arvioinnin.
- Apuvälineitä ja hoitotarvikkeita varten on mahdollista saada lähete sekä perusterveydenhuollosta että erikoissairaanhoidosta. Tarkista paikallinen saatavuus ja jakelun käytänteet.
Hoidon porrastus ja seuranta
- Ks. kaavio virtsankarkailun diagnostiikasta ja hoidosta avoterveydenhuollossa «Naisten virtsankarkailun selvittely avoterveydenhuollossa»1.
- Virtsankarkailun perustutkimukset, hoito ja seuranta voidaan toteuttaa perusterveydenhuollossa.
- Erikoissairaanhoidon konsultaatioon ohjataan, kun virtsankarkailun taustalla epäillään muuta sairautta tai perusterveydenhuollon hoidot ovat riittämättömiä. Malli lähetteestä erikoissairaanhoitoon esitetään lisätietoaineistossa «Malli lähetteestä erikoissairaanhoitoon virtsankarkailun vuoksi»19.
- Virtsankarkailun konservatiivisen hoidon ohjauksen voi antaa asiaan perehtynyt terveydenhuollon ammattihenkilö.
Suomalaisen Lääkäriseuran Duodecimin ja Suomen Gynekologiyhdistyksen asettama työryhmä
Virtsankarkailu (naiset) -suosituksen historiatiedot «Virtsankarkailu (naiset), Käypä hoito -suosituksen historiatiedot»20
Puheenjohtaja:
Tomi Mikkola, LT, professori, ylilääkäri, synnytysten ja naistentautien erikoislääkäri, urogynekologian lisäkoulutus; HUS Naistenklinikka ja Helsingin yliopisto
Kokoava kirjoittaja:
Seija Ala-Nissilä, LT, dosentti, naistentautien ja synnytysten sekä gynekologisen endoskopian erikoislääkäri; Tyks Naistenklinikka ja Turun yliopisto
Jäsenet:
Olavi Airaksinen, fysiatrian professori, ylilääkäri, fysiatrian erikoislääkäri, kivunhoidon ja kuntoutuksen erityispätevyys; KYS:n fysiatrian klinikka ja Itä-Suomen yliopisto
Pauliina Aukee, LT, osastonylilääkäri, synnytysten ja naistentautien erikoislääkäri, urogynekologian ja lääkärikouluttajan erityispätevyys; Keski-Suomen keskussairaalan synnytys- ja naistentautien sekä lantionpohjan tutkimus- ja hoitoyksikkö
Sanna Hallamies, LT, urologian erikoislääkäri, urologisen onkologian lisäkoulutus; HUS Vatsakeskus, urologian linja
Tuija Nieminen, kätilö/sairaanhoitaja (AMK), uroterapeutin kliininen erikoistumiskoulutus; HUS Naistenklinikka, naistentaudit ja synnytykset
Maria Nuotio, LT, geriatrian professori ja ylilääkäri, geriatrian ja yleislääketieteen erikoislääkäri, muistisairauksien erityispätevyys; Turun yliopisto ja Tyks, geriatrian vastuualue
Kaisa Raatikainen, LT, dosentti, naistentautien ja synnytysten erikoislääkäri, urogynekologian lisäkoulutus, kliininen opettaja; Itä-Suomen yliopisto ja KYS
Aleksi Raudasoja, LT, Käypä hoito -toimittaja; Suomalainen Lääkäriseura Duodecim
Minna Törnävä, TtT, fysioterapeutti, seksuaaliterapeutti (NACS), tutkintovastaava, lehtori ylemmät ammattikorkeakoulututkinnot; Tampereen ammattikorkeakoulu, sosiaali- ja terveysala
Sidonnaisuudet
Sidonnaisuusilmoitukset on kerätty 31.3.2026 julkaistun suosituksen laatimisen yhteydessä.
Olavi Airaksinen: Sivutoimet: konsultoiva lääkäri; Respecta Oy. Yksityisvastaanotot: Terveystalo Oy ja Pihlajalinna Oy. Tutkimus- ja kehitystyö: lääketutkimus: GSK. Koulutustoiminta: luentoja: Fysioline Oy, Viatris Oy, Pfizer Oy, Amgen Oy. Kongressit ja seminaarit: Amgen. Luottamustoimet terveydenhuollon alalla: Duodecim valtuuskunnan jäsen. Toiminta terveydenhuollon ohjaukseen pyrkivissä hankkeissa: STM:n työryhmiä: Kunfo, kuntoutuksen uudistamiskomitean työryhmät, kuntoutuksen saatavuusperiaatteet.
Seija Ala-Nissilä: Sivutoimet: kliininen opettaja, osa-aikainen; Turun yliopisto, tohtoritoimikunnan jäsen; Turun yliopisto, yksityislääkäri; Aava ja Mehiläinen Turku. Koulutustoiminta: Pierre Fabre Pharma Norden.
Pauliina Aukee: Sivutoimet: erikoislääkäri; Terveystalo Jyväskylä. Koulutustoiminta: Bayer luentopalkkio. Luottamustoimet terveydenhuollon alalla: Keski-Suomen lääkäriyhdistyksen hallituksen jäsen, Suomen gynekologiyhdistyksen hallituksen jäsen 11/2025 asti.
Sanna Hallamies: Sivutoimet: urologian erikoislääkäri (ammatinharjoittaja); Mehiläinen. Koulutustoiminta: Johnson&Johnson (asiantuntija- ja luentopalkkio), Bayer (asiantuntijapalkkio), Merck (luentopalkkio), Astellas (luentopalkkio). Kongressit ja seminaarit: Johnson&Johnson (kongressimatka), Pierre Fabre (kongressimatka). Luottamustoimet terveydenhuollon alalla: Scandinavian Association of Urology, LUTD collaboration group (jäsen).
Tomi Mikkola: Sivutoimet: professori; HY, yksityislääkäritoiminta Eiran Sairaala, Aava. Koulutustoiminta: Astellas Pharma, Axonics, Bayer, Theramex.
Tuija Nieminen: Ei aiheeseen liittyviä sidonnaisuuksia.
Maria Nuotio: Sivutoimet: ylilääkäri; Turun yliopistollinen sairaala (Tyks), geriatrian vastuualue. Koulutustoiminta: Professio, Amgen, Nutricia, Ontex, Fispen ry, Luustoliitto ry, Suomen Geriatrit ry Luottamustoimet terveydenhuollon alalla: UEMS -geriatrian osasto, Suomen edustaja; Lääkäriliitto, muistisairauksien erityispätevyystoimikunta; Alzheimer tutkimusseura, hallituksen jäsen; Fispen ry, puheenjohtaja; Espen, Council, jäsen; STM, Koti- ja vapaa-ajan tapaturmien ehkäisyn koordinaatioryhmä; FFN (Fragility Fracture Network), Scientific Committee, Steering Committee; EuGMS (European Geriatric Medicine Society), SIG (Special Interest Group), Urinary incontinence, Co-chair.
Kaisa Raatikainen: Kongressit ja seminaarit: Gedeon Richter. Luottamustoimet terveydenhuollon alalla: Suomen Gynekologiyhdistys, urogynekologinen pientyöryhmä.
Aleksi Raudasoja: Sivutoimet: päivystystyö; Pihlajalinna ja Med Group, ammatinharjoittaja; Pihlajalinna, Mehiläinen. Tutkimus- ja kehitystyö: Strategisen tutkimuksen neuvosto.
Minna Törnävä: Sivutoimet: tutkija; Pirkanmaan hyvinvointialue, fysioterapeutti, seksuaaliterapeutti; Terveystalo Tampere. Luottamustoimet terveydenhuollon alalla: Hoitotyön tutkimussäätiö, Hotus (vuodesta 2025); Aikuisten virtsatieinfektioiden ehkäisyn omahoito päivitys, Hotus-hoitosuositustyöryhmän jäsen, Suomen Seksologinen Seura (2023–2025), varapuheenjohtaja sekä tiede- ja tutkimusjaoston jäsen.
Kirjallisuusviite
Virtsankarkailu (naiset). Käypä hoito -suositus. Suomalaisen Lääkäriseuran Duodecimin ja Suomen Gynekologiyhdistyksen asettama työryhmä. Helsinki: Suomalainen Lääkäriseura Duodecim, 2026 (viitattu pp.kk.vvvv). Saatavilla internetissä: www.kaypahoito.fi
Tarkemmat viittausohjeet: «http://www.kaypahoito.fi/web/kh/viittaaminen»4
Vastuun rajaus
Käypä hoito -suositukset ja Vältä viisaasti -suositukset ovat asiantuntijoiden laatimia yhteenvetoja yksittäisten sairauksien diagnostiikan ja hoidon vaikuttavuudesta. Suositukset toimivat lääkärin tai muun terveydenhuollon ammattilaisen päätöksenteon tukena hoitopäätöksiä tehtäessä. Ne eivät korvaa lääkärin tai muun terveydenhuollon ammattilaisen omaa arviota yksittäisen potilaan parhaasta mahdollisesta diagnostiikasta, hoidosta ja kuntoutuksesta hoitopäätöksiä tehtäessä.
Tiedonhakukäytäntö
Systemaattinen kirjallisuushaku on hoitosuosituksen perusta. Lue lisää artikkelista khk00007
Kirjallisuutta
- Haylen BT, de Ridder D, Freeman RM, ym. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Neurourol Urodyn 2010;29(1):4-20 «PMID: 19941278»PubMed
- Hunskaar S, Burgio K, Diokno A, ym. Epidemiology and natural history of urinary incontinence in women. Urology 2003;62(4 Suppl 1):16-23 «PMID: 14550833»PubMed
- Cerruto MA, D'Elia C, Aloisi A, ym. Prevalence, incidence and obstetric factors' impact on female urinary incontinence in Europe: a systematic review. Urol Int 2013;90(1):1-9 «PMID: 22868349»PubMed
- Schreiber Pedersen L, Lose G, Høybye MT, ym. Prevalence of urinary incontinence among women and analysis of potential risk factors in Germany and Denmark. Acta Obstet Gynecol Scand 2017;96(8):939-948 «PMID: 28401541»PubMed
- Hannestad YS, Rortveit G, Sandvik H, ym. A community-based epidemiological survey of female urinary incontinence: the Norwegian EPINCONT study. Epidemiology of Incontinence in the County of Nord-Trøndelag. J Clin Epidemiol 2000;53(11):1150-7 «PMID: 11106889»PubMed
- Jahanlu D, Hunskaar S. The Hordaland Women's Cohort: prevalence, incidence, and remission of urinary incontinence in middle-aged women. Int Urogynecol J 2010;21(10):1223-9 «PMID: 20449565»PubMed
- Rortveit G, Hannestad YS, Daltveit AK, ym. Age- and type-dependent effects of parity on urinary incontinence: the Norwegian EPINCONT study. Obstet Gynecol 2001;98(6):1004-10 «PMID: 11755545»PubMed
- Matthews CA, Whitehead WE, Townsend MK, ym. Risk factors for urinary, fecal, or dual incontinence in the Nurses' Health Study. Obstet Gynecol 2013;122(3):539-45 «PMID: 23921863»PubMed
- Maggi S, Minicuci N, Langlois J, ym. Prevalence rate of urinary incontinence in community-dwelling elderly individuals: the Veneto study. J Gerontol A Biol Sci Med Sci 2001;56(1):M14-8 «PMID: 11193226»PubMed
- Ostaszkiewicz J, Johnston L, Roe B. Timed voiding for the management of urinary incontinence in adults. Cochrane Database Syst Rev 2004;2004(1):CD002802 «PMID: 14973993»PubMed
- Buckley BS, Lapitan MC, Epidemiology Committee of the Fourth International Consultation on Incontinence, Paris, 2008. Prevalence of urinary incontinence in men, women, and children--current evidence: findings of the Fourth International Consultation on Incontinence. Urology 2010;76(2):265-70 «PMID: 20541241»PubMed
- Wennberg AL, Molander U, Fall M, ym. A longitudinal population-based survey of urinary incontinence, overactive bladder, and other lower urinary tract symptoms in women. Eur Urol 2009;55(4):783-91 «PMID: 19157689»PubMed
- Sundqvist C, Li X, Sundquist K, ym. Sociodemographic Disparities and Parity in Relation to Urinary Incontinence: A Nationwide Primary Healthcare Cohort Study (1997-2018). J Clin Med 2022;11(3): «PMID: 35159948»PubMed
- Abufaraj M, Xu T, Cao C, ym. Prevalence and trends in urinary incontinence among women in the United States, 2005-2018. Am J Obstet Gynecol 2021;225(2):166.e1-166.e12 «PMID: 33727114»PubMed
- Shang X, Fu Y, Jin X, ym. Association of overweight, obesity and risk of urinary incontinence in middle-aged and older women: a meta epidemiology study. Front Endocrinol (Lausanne) 2023;14():1220551 «PMID: 37886637»PubMed
- Choi JM, Jiang J, Chang J, ym. Impact of Lifetime Obesity on Urinary Incontinence in the Women's Health Initiative. J Urol 2022;207(5):1096-1104 «PMID: 34967666»PubMed
- Hagen S, Sellers C, Elders A, ym. Urinary incontinence, faecal incontinence and pelvic organ prolapse symptoms 20-26 years after childbirth: A longitudinal cohort study. BJOG 2024;131(13):1815-1823 «PMID: 39079703»PubMed
- Wesnes SL, Hunskaar S, Bo K, ym. The effect of urinary incontinence status during pregnancy and delivery mode on incontinence postpartum. A cohort study. BJOG 2009;116(5):700-7 «PMID: 19220234»PubMed
- Ebbesen MH, Hannestad YS, Midthjell K, ym. Diabetes and urinary incontinence − prevalence data from Norway. Acta Obstet Gynecol Scand 2007;86(10):1256-62 «PMID: 17851814»PubMed
- Danforth KN, Townsend MK, Curhan GC, ym. Type 2 diabetes mellitus and risk of stress, urge and mixed urinary incontinence. J Urol 2009;181(1):193-7 «PMID: 19013621»PubMed
- Løwenstein E, Jepsen R, Andersen LL, ym. Prevalence of urinary incontinence among women with diabetes in the Lolland-Falster Health Study, Denmark. Neurourol Urodyn 2021;40(3):855-867 «PMID: 33645842»PubMed
- Rortveit G, Daltveit AK, Hannestad YS, ym. Urinary incontinence after vaginal delivery or cesarean section. N Engl J Med 2003;348(10):900-7 «PMID: 12621134»PubMed
- Tähtinen RM, Cartwright R, Tsui JF, ym. Long-term Impact of Mode of Delivery on Stress Urinary Incontinence and Urgency Urinary Incontinence: A Systematic Review and Meta-analysis. Eur Urol 2016;70(1):148-158 «PMID: 26874810»PubMed
- Humalajärvi N, Aukee P, Kairaluoma MV, ym. Quality of life and pelvic floor dysfunction symptoms after hysterectomy with or without pelvic organ prolapse. Eur J Obstet Gynecol Reprod Biol 2014;182():16-21 «PMID: 25218547»PubMed
- Christoffersen NM, Klarskov N, Gradel KO, ym. Increased risk of stress urinary incontinence surgery after hysterectomy for benign indication-a population-based cohort study. Am J Obstet Gynecol 2023;229(2):149.e1-149.e9 «PMID: 37116821»PubMed
- Bardino M, Di Martino M, Ricci E, ym. Frequency and Determinants of Urinary Incontinence in Adolescent and Young Nulliparous Women. J Pediatr Adolesc Gynecol 2015;28(6):462-70 «PMID: 26233290»PubMed
- Koskimäki J, Hakama M, Huhtala H, ym. Association of non-urological diseases with lower urinary tract symptoms. Scand J Urol Nephrol 2001;35(5):377-81 «PMID: 11771864»PubMed
- Bertuit J, Bakker E, Rejano-Campo M. Relationship between urinary incontinence and back or pelvic girdle pain: a systematic review with meta-analysis. Int Urogynecol J 2021;32(5):1073-1086 «PMID: 33620534»PubMed
- Welk B, Baverstock R. Is there a link between back pain and urinary symptoms? Neurourol Urodyn 2020;39(2):523-532 «PMID: 31899561»PubMed
- Townsend MK, Jura YH, Curhan GC, ym. Fluid intake and risk of stress, urgency, and mixed urinary incontinence. Am J Obstet Gynecol 2011;205(1):73.e1-6 «PMID: 21481835»PubMed
- Imamura M, Williams K, Wells M, ym. Lifestyle interventions for the treatment of urinary incontinence in adults. Cochrane Database Syst Rev 2015;2015(12):CD003505 «PMID: 26630349»PubMed
- Faiena I, Patel N, Parihar JS, ym. Conservative Management of Urinary Incontinence in Women. Rev Urol 2015;17(3):129-39 «PMID: 26543427»PubMed
- Jura YH, Townsend MK, Curhan GC, ym. Caffeine intake, and the risk of stress, urgency and mixed urinary incontinence. J Urol 2011;185(5):1775-80 «PMID: 21420114»PubMed
- Hirayama F, Lee AH. Green tea drinking is inversely associated with urinary incontinence in middle-aged and older women. Neurourol Urodyn 2011;30(7):1262-5 «PMID: 21404319»PubMed
- Sun S, Liu D, Jiao Z. Coffee and caffeine intake and risk of urinary incontinence: a meta-analysis of observational studies. BMC Urol 2016;16(1):61 «PMID: 27716171»PubMed
- Tähtinen RM, Auvinen A, Cartwright R, ym. Smoking and bladder symptoms in women. Obstet Gynecol 2011;118(3):643-648 «PMID: 21860295»PubMed
- Kawahara T, Ito H, Yao M, ym. Impact of smoking habit on overactive bladder symptoms and incontinence in women. Int J Urol 2020;27(12):1078-1086 «PMID: 32875688»PubMed
- Michel KF, Rangnekar AN, Slinger M, ym. Association of Smoking Status and Pack Year History With Urinary Urgency Symptoms. Neurourol Urodyn 2024;43(8):1842-1849 «PMID: 39268788»PubMed
- Townsend MK, Danforth KN, Rosner B, ym. Physical activity and incident urinary incontinence in middle-aged women. J Urol 2008;179(3):1012-6; discussion 1016-7 «PMID: 18206951»PubMed
- Kim MM, Ladi-Seyedian SS, Ginsberg DA, ym. The Association of Physical Activity and Urinary Incontinence in US Women: Results from a Multi-Year National Survey. Urology 2022;159():72-77 «PMID: 34644590»PubMed
- Laakkonen EK, Kulmala J, Aukee P, ym. Female reproductive factors are associated with objectively measured physical activity in middle-aged women. PLoS One 2017;12(2):e0172054 «PMID: 28225786»PubMed
- Tibaek S, Gard G, Klarskov P, ym. Prevalence of lower urinary tract symptoms (LUTS) in stroke patients: a cross-sectional, clinical survey. Neurourol Urodyn 2008;27(8):763-71 «PMID: 18551565»PubMed
- Sakakibara R, Uchiyama T, Yamanishi T, ym. Dementia and lower urinary dysfunction: with a reference to anticholinergic use in elderly population. Int J Urol 2008;15(9):778-88 «PMID: 18643858»PubMed
- de Sèze M, Ruffion A, Denys P, ym. The neurogenic bladder in multiple sclerosis: review of the literature and proposal of management guidelines. Mult Scler 2007;13(7):915-28 «PMID: 17881401»PubMed
- Li FF, Cui YS, Yan R, ym. Prevalence of lower urinary tract symptoms, urinary incontinence and retention in Parkinson's disease: A systematic review and meta-analysis. Front Aging Neurosci 2022;14():977572 «PMID: 36172485»PubMed
- Ransmayr GN, Holliger S, Schletterer K, ym. Lower urinary tract symptoms in dementia with Lewy bodies, Parkinson disease, and Alzheimer disease. Neurology 2008;70(4):299-303 «PMID: 18209204»PubMed
- DuBeau CE, Kuchel GA, Johnson T 2nd, ym. Incontinence in the frail elderly: report from the 4th International Consultation on Incontinence. Neurourol Urodyn 2010;29(1):165-78 «PMID: 20025027»PubMed
- Schröder A, Abrams P, Andersson KE ym. Urinary incontinence in frail/older men and women. Guidelines on urinary incontinence. European Association of Urology 2010. http://www.uroweb.org/gls/pockets/english/Urinary%20Incontinence%202010.pdf
- Klovning A, Hunskaar S, Eriksen BC. Validity of a scored urological history in detecting detrusor instability in female urinary incontinence. Acta Obstet Gynecol Scand 1996;75(10):941-5 «PMID: 9003097»PubMed
- Nambiar AK, Arlandis S, Bø K, ym. European Association of Urology Guidelines on the Diagnosis and Management of Female Non-neurogenic Lower Urinary Tract Symptoms. Part 1: Diagnostics, Overactive Bladder, Stress Urinary Incontinence, and Mixed Urinary Incontinence. Eur Urol 2022;82(1):49-59 «PMID: 35216856»PubMed
- Virtsatieinfektiot. Käypä hoito -suositus. Suomalaisen Lääkäriseuran Duodecimin, Suomen Nefrologiyhdistys ry:n, Kliiniset mikrobiologit ry:n, Suomen Infektiolääkärit ry:n, Suomen Kliinisen Kemian Erikoislääkäriyhdistys ry:n, Suomen Lastenlääkäriyhdistys ry:n, Suomen Urologiyhdistyksen ja Suomen yleislääketieteen yhdistys ry:n asettama työryhmä. Helsinki: Suomalainen Lääkäriseura Duodecim, 2024 (viitattu pp.kk.vvvv). Saatavilla internetissä: www.kaypahoito.fi
- Rife CC, Farrow GM, Utz DC. Urine cytology of transitional cell neoplasms. Urol Clin North Am 1979;6(3):599-612 «PMID: 505675»PubMed
- Koss LG, Deitch D, Ramanathan R, ym. Diagnostic value of cytology of voided urine. Acta Cytol 1985;29(5):810-6 «PMID: 3863429»PubMed
- Chahal R, Gogoi NK, Sundaram SK. Is it necessary to perform urine cytology in screening patients with haematuria? Eur Urol 2001;39(3):283-6 «PMID: 11275720»PubMed
- Goode PS, Locher JL, Bryant RL, ym. Measurement of postvoid residual urine with portable transabdominal bladder ultrasound scanner and urethral catheterization. Int Urogynecol J Pelvic Floor Dysfunct 2000;11(5):296-300 «PMID: 11052565»PubMed
- Bernstein IT. The pelvic floor muscles: muscle thickness in healthy and urinary-incontinent women measured by perineal ultrasonography with reference to the effect of pelvic floor training. Estrogen receptor studies. Neurourol Urodyn 1997;16(4):237-75 «PMID: 9220475»PubMed
- Dietz HP, Wilson PD, Clarke B. The use of perineal ultrasound to quantify levator activity and teach pelvic floor muscle exercises. Int Urogynecol J Pelvic Floor Dysfunct 2001;12(3):166-8; discussion 168-9 «PMID: 11451004»PubMed
- Kociszewski J, Rautenberg O, Kuszka A, ym. Can we place tension-free vaginal tape where it should be? The one-third rule. Ultrasound Obstet Gynecol 2012;39(2):210-4 «PMID: 21793084»PubMed
- Haylen BT, Maher CF, Barber MD, ym. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic organ prolapse (POP). Int Urogynecol J 2016;27(4):655-84 «PMID: 26984443»PubMed
- Tunn R, Schaer G, Peschers U, ym. Updated recommendations on ultrasonography in urogynecology. Int Urogynecol J Pelvic Floor Dysfunct 2005;16(3):236-41 «PMID: 15875241»PubMed
- Virtanen HS, Kiilholma P. Urogynecologic ultrasound is a useful aid in the assessment of female stress urinary incontinence--a prospective study with TVT procedure. Int Urogynecol J Pelvic Floor Dysfunct 2002;13(4):218-22; discussion 223 «PMID: 12189426»PubMed
- Dalpiaz O, Curti P. Role of perineal ultrasound in the evaluation of urinary stress incontinence and pelvic organ prolapse: a systematic review. Neurourol Urodyn 2006;25(4):301-6; discussion 307 «PMID: 16688711»PubMed
- Kirschner-Hermanns R, Fielding JR, Versi E, ym. Magnetic resonance imaging of the lower urinary tract. Curr Opin Obstet Gynecol 1997;9(5):317-9 «PMID: 9360814»PubMed
- Rinne K, Kainulainen S, Aukee S, ym. Dynamic MRI confirms support of the mid-urethra by TVT and TVT-O surgery for stress incontinence. Acta Obstet Gynecol Scand 2011;90(6):629-35 «PMID: 21382017»PubMed
- Gilleran JP, Zimmern P. An evidence-based approach to the evaluation and management of stress incontinence in women. Curr Opin Urol 2005;15(4):236-43 «PMID: 15928512»PubMed
- Lihavuus (lapset, nuoret ja aikuiset). Käypä hoito -suositus. Suomalaisen Lääkäriseuran Duodecimin, Suomen Lihavuustutkijat ry:n ja Suomen Lastenlääkäriyhdistys ry:n asettama työryhmä. Helsinki: Suomalainen Lääkäriseura Duodecim, 2025 (viitattu pp.kk.vvvv). Saatavilla internetissä: www.kaypahoito.fi
- Tupakka- ja nikotiiniriippuvuuden ehkäisy ja hoito. Käypä hoito -suositus. Suomalaisen Lääkäriseuran Duodecimin ja Suomen Yleislääketieteen yhdistyksen asettama työryhmä. Helsinki: Suomalainen Lääkäriseura Duodecim, 2024 (viitattu pp.kk.vvvv). Saatavilla internetissä: www.kaypahoito.fi
- Linneberg S, Leenskjold S, Glavind K. A five year follow-up of women with obstetric anal sphincter rupture at their first delivery. Eur J Obstet Gynecol Reprod Biol 2016;203():315-9 «PMID: 27423529»PubMed
- Brown SJ, Gartland D, Donath S, ym. Effects of prolonged second stage, method of birth, timing of caesarean section and other obstetric risk factors on postnatal urinary incontinence: an Australian nulliparous cohort study. BJOG 2011;118(8):991-1000 «PMID: 21489125»PubMed
- Leenskjold S, Høj L, Pirhonen J. Manual protection of the perineum reduces the risk of obstetric anal sphincter ruptures. Dan Med J 2015;62(5): «PMID: 26050831»PubMed
- Jiang H, Qian X, Carroli G, ym. Selective versus routine use of episiotomy for vaginal birth. Cochrane Database Syst Rev 2017;2(2):CD000081 «PMID: 28176333»PubMed
- Okeahialam NA, Sultan AH, Thakar R. The prevention of perineal trauma during vaginal birth. Am J Obstet Gynecol 2024;230(3S):S991-S1004 «PMID: 37635056»PubMed
- Hannestad YS, Rortveit G, Daltveit AK, ym. Are smoking and other lifestyle factors associated with female urinary incontinence? The Norwegian EPINCONT Study. BJOG 2003;110(3):247-54 «PMID: 12628262»PubMed
- Wallace SA, Roe B, Williams K, ym. Bladder training for urinary incontinence in adults. Cochrane Database Syst Rev 2004;2004(1):CD001308 «PMID: 14973967»PubMed
- Füsgen I, Wiedemann A. [Chronic Constipation: A Geriatric Syndrome with Urological Implications]. Aktuelle Urol 2016;47(1):51-3 «PMID: 26574951»PubMed
- Hendriks EJ, Kessels AG, de Vet HC, ym. Prognostic indicators of poor short-term outcome of physiotherapy intervention in women with stress urinary incontinence. Neurourol Urodyn 2010;29(3):336-43 «PMID: 19475574»PubMed
- Hou Y, Feng S, Tong B, ym. Effect of pelvic floor muscle training using mobile health applications for stress urinary incontinence in women: a systematic review. BMC Womens Health 2022;22(1):400 «PMID: 36192744»PubMed
- de Araujo CC, Brito LGO, Marques AA, ym. Use of a Mobile Application for Pelvic Floor Muscle Training in Women With Urinary Incontinence: a Randomized Control Trial. Int Urogynecol J 2024;35(3):589-598 «PMID: 38214718»PubMed
- Wadensten T, Nyström E, Franzén K, ym. A Mobile App for Self-management of Urgency and Mixed Urinary Incontinence in Women: Randomized Controlled Trial. J Med Internet Res 2021;23(4):e19439 «PMID: 33818395»PubMed
- Cody JD, Jacobs ML, Richardson K, ym. Oestrogen therapy for urinary incontinence in post-menopausal women. Cochrane Database Syst Rev 2012;10(10):CD001405 «PMID: 23076892»PubMed
- Ewies AA, Alfhaily F. Topical vaginal estrogen therapy in managing postmenopausal urinary symptoms: a reality or a gimmick? Climacteric 2010;13(5):405-18 «PMID: 20670198»PubMed
- Cardozo L, Lose G, McClish D, ym. A systematic review of the effects of estrogens for symptoms suggestive of overactive bladder. Acta Obstet Gynecol Scand 2004;83(10):892-7 «PMID: 15453881»PubMed
- Rahn DD, Carberry C, Sanses TV, ym. Vaginal estrogen for genitourinary syndrome of menopause: a systematic review. Obstet Gynecol 2014;124(6):1147-1156 «PMID: 25415166»PubMed
- Te West NID, Harris K, Jeffrey S, ym. The effect of 12 weeks of estriol cream on stress urinary incontinence post-menopause: A prospective multinational observational study. Neurourol Urodyn 2023;42(4):799-806 «PMID: 36840920»PubMed
- Nemirovsky A, Villela NA, Yuan JC, ym. Vaginal Hormone Therapy for Conditions of the Lower Urinary Tract. Curr Urol Rep 2023;24(2):41-50 «PMID: 36454371»PubMed
- Collà Ruvolo C, Gabrielli O, Formisano C, ym. Prasterone in the treatment of mild to moderate urge incontinence: an observational study. Menopause 2022;29(8):957-962 «PMID: 35881944»PubMed
- Ren C, Qiang Z. Topical estrogen therapy ameliorates bladder estrogen receptor β expression in female patients with overactive bladder. Am J Transl Res 2023;15(12):6849-6857 «PMID: 38186992»PubMed
- McVicker L, Labeit AM, Coupland CAC, ym. Vaginal Estrogen Therapy Use and Survival in Females With Breast Cancer. JAMA Oncol 2024;10(1):103-108 «PMID: 37917089»PubMed
- Tiitinen A, Kero K. Paikallisestrogeenit ja rintasyöpä. Suom lääkäril 2020;75(3):117-121
- Vaihdevuodet. Käypä hoito -suositus. Suomalaisen Lääkäriseuran Duodecimin, Suomen Gynekologiyhdistys ry:n ja Suomen Menopaussitutkimusseura ry:n asettama työryhmä. Helsinki: Suomalainen Lääkäriseura Duodecim, 2025 (viitattu pp.kk.vvvv). Saatavilla internetissä: www.kaypahoito.fi
- Rahkola-Soisalo P, Savolainen-Peltonen H, Gissler M, ym. Increased risk for stress urinary incontinence in women with postmenopausal hormone therapy. Int Urogynecol J 2019;30(2):251-256 «PMID: 29946829»PubMed
- Pautasso S, Mancarella M, Novara L, ym. Intravaginal prasterone for urinary urgency in postmenopausal women without urodynamic detrusor overactivity. Maturitas 2025;199():108620 «PMID: 40449177»PubMed
- Misasi G, Russo E, Montt Guevara MM, ym. Effects of vaginal DHEA on stress urinary incontinence in postmenopausal women with vulvovaginal atrophy. Maturitas 2025;196():108232 «PMID: 40068355»PubMed
- Collà Ruvolo C, Ursino M, Formisano C, ym. Urodynamic evaluation of prasterone vaginal treatment of mild to moderate urge incontinence in women with vulvovaginal atrophy: multicenter prospective study. Menopause 2025;32(5):428-432 «PMID: 39933040»PubMed
- Rubin R, Sanaee M, Yee A, ym. Prevalence of urinary tract infections in women with vulvovaginal atrophy and the impact of vaginal prasterone on the rate of urinary tract infections. Menopause 2025;32(3):217-227 «PMID: 39774900»PubMed
- Dey A, Georgiadis G, Umezurike J, ym. Mirabegron Versus Placebo and Other Therapeutic Modalities in the Treatment of Patients with Overactive Bladder Syndrome-A Systematic Review. Eur Urol Focus 2025;11(2):323-336 «PMID: 39343691»PubMed
- Irwin DE, Milsom I, Chancellor MB, ym. Dynamic progression of overactive bladder and urinary incontinence symptoms: a systematic review. Eur Urol 2010;58(4):532-43 «PMID: 20573443»PubMed
- Khullar V, Rahnama'i MS, Veit-Rubin N, ym. Can we harness the placebo effect to improve care in lower urinary tract dysfunction? ICI-RS 2019. Neurourol Urodyn 2020;39 Suppl 3():S80-S87 «PMID: 32311166»PubMed
- Herbison P, McKenzie JE. Which anticholinergic is best for people with overactive bladders? A network meta-analysis. Neurourol Urodyn 2019;38(2):525-534 «PMID: 30575999»PubMed
- Zhang J, Chi J, Lou K, ym. Comparison of efficacy and safety of mirabegron and vibegron in the treatment of Overactive Bladder (OAB) in older women: A systematic review and meta-analysis. PLoS One 2025;20(4):e0317550 «PMID: 40198627»PubMed
- Chapple CR, Cruz F, Cardozo L, ym. Safety and Efficacy of Mirabegron: Analysis of a Large Integrated Clinical Trial Database of Patients with Overactive Bladder Receiving Mirabegron, Antimuscarinics, or Placebo. Eur Urol 2020;77(1):119-128 «PMID: 31635815»PubMed
- Madersbacher H, Mürtz G, Stöhrer M. Neurogenic detrusor overactivity in adults: a review on efficacy, tolerability and safety of oral antimuscarinics. Spinal Cord 2013;51(6):432-41 «PMID: 23743498»PubMed
- Amundsen CL, Richter HE, Menefee SA, ym. OnabotulinumtoxinA vs Sacral Neuromodulation on Refractory Urgency Urinary Incontinence in Women: A Randomized Clinical Trial. JAMA 2016;316(13):1366-1374 «PMID: 27701661»PubMed
- Amundsen CL, Komesu YM, Chermansky C, ym. Two-Year Outcomes of Sacral Neuromodulation Versus OnabotulinumtoxinA for Refractory Urgency Urinary Incontinence: A Randomized Trial. Eur Urol 2018;74(1):66-73 «PMID: 29482936»PubMed
- Drake MJ, Nitti VW, Ginsberg DA, ym. Comparative assessment of the efficacy of onabotulinumtoxinA and oral therapies (anticholinergics and mirabegron) for overactive bladder: a systematic review and network meta-analysis. BJU Int 2017;120(5):611-622 «PMID: 28670786»PubMed
- Campbell JD, Gries KS, Watanabe JH, ym. Treatment success for overactive bladder with urinary urge incontinence refractory to oral antimuscarinics: a review of published evidence. BMC Urol 2009;9():18 «PMID: 19930578»PubMed
- Edlund C, Peeker R, Fall M. Clam ileocystoplasty: successful treatment of severe bladder overactivity. Scand J Urol Nephrol 2001;35(3):190-5 «PMID: 11487070»PubMed
- Luangkhot R, Peng BC, Blaivas JG. Ileocecocystoplasty for the management of refractory neurogenic bladder: surgical technique and urodynamic findings. J Urol 1991;146(5):1340-4 «PMID: 1942287»PubMed
- Robertson AS, Davies JB, Webb RJ, ym. Bladder augmentation and replacement. Urodynamic and clinical review of 25 patients. Br J Urol 1991;68(6):590-7 «PMID: 1773289»PubMed
- Labrie J, Berghmans BL, Fischer K, ym. Surgery versus physiotherapy for stress urinary incontinence. N Engl J Med 2013;369(12):1124-33 «PMID: 24047061»PubMed
- Itkonen Freitas AM, Mentula M, Rahkola-Soisalo P, ym. Tension-Free Vaginal Tape Surgery versus Polyacrylamide Hydrogel Injection for Primary Stress Urinary Incontinence: A Randomized Clinical Trial. J Urol 2020;203(2):372-378 «PMID: 31479396»PubMed
- Sokol ER, Karram MM, Dmochowski R. Efficacy and safety of polyacrylamide hydrogel for the treatment of female stress incontinence: a randomized, prospective, multicenter North American study. J Urol 2014;192(3):843-9 «PMID: 24704117»PubMed
- Lamblin G, Boix S, Moret S, ym. Effectiveness and Safety Profile of Urethral Bulking with Bulkamid(®) for Stress Urinary Incontinence: A French Multi-Center Cohort Study. Int Urogynecol J 2025;36(1):205-211 «PMID: 39656238»PubMed
- Freitas AI, Isaksson C, Rahkola-Soisalo P, ym. Tension-Free Vaginal Tape versus Polyacrylamide Hydrogel Injection for Stress Urinary Incontinence - 5-Year Follow-Up. NEJM Evid 2025;4(5):EVIDoa2400216 «PMID: 40261117»PubMed
- Svenningsen R, Oversand SH, Schiøtz HA, ym. Comparing risk of repeat surgery for stress urinary incontinence after mid-urethral slings and polyacrylamide hydrogel. Acta Obstet Gynecol Scand 2021;100(12):2186-2192 «PMID: 34622944»PubMed
- Ulmsten U, Falconer C, Johnson P, ym. A multicenter study of tension-free vaginal tape (TVT) for surgical treatment of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 1998;9(4):210-3 «PMID: 9795826»PubMed
- Clement KD, Lapitan MC, Omar MI, ym. Urodynamic studies for management of urinary incontinence in children and adults: A short version Cochrane systematic review and meta-analysis. Neurourol Urodyn 2015;34(5):407-12 «PMID: 24853652»PubMed
- Zyczynski HM, Albo ME, Goldman HB, ym. Change in Overactive Bladder Symptoms After Surgery for Stress Urinary Incontinence in Women. Obstet Gynecol 2015;126(2):423-430 «PMID: 26241434»PubMed
- Jha S, Jeppson PC, Dokmeci F, ym. Management of mixed urinary incontinence: IUGA committee opinion. Int Urogynecol J 2024;35(2):291-301 «PMID: 38252279»PubMed
- Richter HE, Diokno A, Kenton K, ym. Predictors of treatment failure 24 months after surgery for stress urinary incontinence. J Urol 2008;179(3):1024-30 «PMID: 18206917»PubMed
- Ruffolo AF, Lallemant M, Garabedian C, ym. The impact of pregnancy and childbirth on stress urinary incontinence in women previously submitted to mid-urethral sling: A systematic review and metanalysis. Neurourol Urodyn 2024;43(7):1631-1646 «PMID: 38725418»PubMed
- Maher C, Feiner B, Baessler K, ym. Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev 2013;(4):CD004014 «PMID: 23633316»PubMed
- Khayyami Y, Elmelund M, Lose G, ym. De novo urinary incontinence after pelvic organ prolapse surgery-a national database study. Int Urogynecol J 2020;31(2):305-308 «PMID: 31302717»PubMed
- Borstad E, Abdelnoor M, Staff AC, ym. Surgical strategies for women with pelvic organ prolapse and urinary stress incontinence. Int Urogynecol J 2010;21(2):179-86 «PMID: 19940978»PubMed
- Lensen EJ, Withagen MI, Kluivers KB, ym. Urinary incontinence after surgery for pelvic organ prolapse. Neurourol Urodyn 2013;32(5):455-9 «PMID: 23024012»PubMed
- Richter HE, Litman HJ, Lukacz ES, ym. Demographic and clinical predictors of treatment failure one year after midurethral sling surgery. Obstet Gynecol 2011;117(4):913-921 «PMID: 21422865»PubMed
- Hellberg D, Holmgren C, Lanner L, ym. The very obese woman and the very old woman: tension-free vaginal tape for the treatment of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 2007;18(4):423-9 «PMID: 16868657»PubMed
- Nager CW, Sirls L, Litman HJ, ym. Baseline urodynamic predictors of treatment failure 1 year after mid urethral sling surgery. J Urol 2011;186(2):597-603 «PMID: 21683412»PubMed
- Braga A, Caccia G, Papadia A, ym. Urethral bulking agents for the treatment of recurrent stress urinary incontinence: A systematic review and meta-analysis. Maturitas 2022;163():28-37 «PMID: 35679770»PubMed
- Bakali E, Buckley BS, Hilton P, ym. Treatment of recurrent stress urinary incontinence after failed minimally invasive synthetic suburethral tape surgery in women. Cochrane Database Syst Rev 2013;(2):CD009407 «PMID: 23450602»PubMed
- Ruffolo AF, Melocchi T, Frigerio M, ym. Efficacy and safety of repeated synthetic mid-urethral sling for recurrent stress urinary incontinence: A systematic review and metanalysis. Eur J Obstet Gynecol Reprod Biol 2025;308():34-46 «PMID: 40010159»PubMed
- Lo TS, Horng SG, Chang CL, ym. Tension-free vaginal tape procedure after previous failure in incontinence surgery. Urology 2002;60(1):57-61 «PMID: 12100922»PubMed
- Liapis A, Bakas P, Lazaris D, ym. Tension-free vaginal tape in the management of recurrent stress incontinence. Arch Gynecol Obstet 2004;269(3):205-7 «PMID: 12942265»PubMed
- Goldman HB, Rackley RR, Appell RA. The efficacy of urethrolysis without re-suspension for iatrogenic urethral obstruction. J Urol 1999;161(1):196-8; discussion 198-9 «PMID: 10037397»PubMed
- Danforth KN, Shah AD, Townsend MK, ym. Physical activity and urinary incontinence among healthy, older women. Obstet Gynecol 2007;109(3):721-7 «PMID: 17329526»PubMed
- Visser E, de Bock GH, Messelink EJ, ym. Active encouragement of older women with urinary incontinence in primary care to undergo diagnosis and treatment: a matched-pair cluster randomized controlled trial. Maturitas 2015;80(2):212-9 «PMID: 25534171»PubMed
- Moon S, Chung HS, Kim YJ, ym. The impact of urinary incontinence on falls: A systematic review and meta-analysis. PLoS One 2021;16(5):e0251711 «PMID: 34010311»PubMed
- Gibson W, Johnson T, Kirschner-Hermanns R, ym. Incontinence in frail elderly persons: Report of the 6th International Consultation on Incontinence. Neurourol Urodyn 2021;40(1):38-54 «PMID: 33085806»PubMed
- Monisairas potilas. Käypä hoito -suositus. Suomalaisen Lääkäriseuran Duodecimin ja Suomen yleislääketieteen yhdistyksen asettama työryhmä. Helsinki: Suomalainen Lääkäriseura Duodecim, 2021 (viitattu pp.kk.vvvv). Saatavilla internetissä: www.kaypahoito.fi
- Suominen MH, Jyvakorpi SK, Pitkala KH, ym. Nutritional guidelines for older people in Finland. J Nutr Health Aging 2014;18(10):861-7 «PMID: 25470800»PubMed
- Kim H, Yoshida H, Suzuki T. The effects of multidimensional exercise treatment on community-dwelling elderly Japanese women with stress, urge, and mixed urinary incontinence: a randomized controlled trial. Int J Nurs Stud 2011;48(10):1165-72 «PMID: 21459381»PubMed
- Kim H, Suzuki T, Yoshida Y, ym. Effectiveness of multidimensional exercises for the treatment of stress urinary incontinence in elderly community-dwelling Japanese women: a randomized, controlled, crossover trial. J Am Geriatr Soc 2007;55(12):1932-9 «PMID: 17944890»PubMed
- Engberg S, Sereika SM. Effectiveness of Pelvic Floor Muscle Training for Urinary Incontinence: Comparison Within and Between Nonhomebound and Homebound Older Adults. J Wound Ostomy Continence Nurs 2016;43(3):291-300 «PMID: 27163683»PubMed
- Talley KMC, Wyman JF, Bronas U, ym. Defeating Urinary Incontinence with Exercise Training: Results of a Pilot Study in Frail Older Women. J Am Geriatr Soc 2017;65(6):1321-1327 «PMID: 28248418»PubMed
- Kay GG, Granville LJ. Antimuscarinic agents: implications and concerns in the management of overactive bladder in the elderly. Clin Ther 2005;27(1):127-38; quiz 139-40 «PMID: 15763613»PubMed
- Kraus SR, Bavendam T, Brake T, ym. Vulnerable elderly patients and overactive bladder syndrome. Drugs Aging 2010;27(9):697-713 «PMID: 20809661»PubMed
- Samuelsson E, Odeberg J, Stenzelius K, ym. Effect of pharmacological treatment for urinary incontinence in the elderly and frail elderly: A systematic review. Geriatr Gerontol Int 2015;15(5):521-34 «PMID: 25656412»PubMed
- Stoniute A, Madhuvrata P, Still M, ym. Oral anticholinergic drugs versus placebo or no treatment for managing overactive bladder syndrome in adults. Cochrane Database Syst Rev 2023;5(5):CD003781 «PMID: 37160401»PubMed
- Reinold J, Schäfer W, Christianson L, ym. Anticholinergic Burden and Fractures: A Systematic Review with Methodological Appraisal. Drugs Aging 2020;37(12):885-897 «PMID: 33094444»PubMed
- Muistisairaudet. Käypä hoito -suositus. Suomalaisen Lääkäriseuran Duodecimin, Societas Gerontologica Fennican, Suomen Geriatrit -yhdistyksen, Suomen Neurologisen Yhdistyksen, Suomen Psykogeriatrisen Yhdistyksen ja Suomen Yleislääketieteen yhdistyksen asettama työryhmä. Helsinki: Suomalainen Lääkäriseura Duodecim, 2023 (viitattu 6.2.2026). Saatavilla internetissä: www.kaypahoito.fi
- Parker-Autry CY, Bauer S, Ford C, ym. Examining the Role of Frailty on Treatment Patterns and Complications Among Older Women Undergoing Procedure-Based Treatment for Urinary Incontinence. J Gerontol A Biol Sci Med Sci 2024;79(6): «PMID: 38280028»PubMed
- Kao YL, Ou YC, Kuo HC. Bladder Dysfunction in Older Adults: The Botulinum Toxin Option. Drugs Aging 2022;39(6):401-416 «PMID: 35696022»PubMed
- Malek JM, Ellington DR, Jauk V, ym. The effect of age on stress and urgency urinary incontinence outcomes in women undergoing primary midurethral sling. Int Urogynecol J 2015;26(6):831-5 «PMID: 25510465»PubMed
- Faurie B, Hascoet J, Richard C, ym. Outpatient Periurethral Injections of Polyacrylamide Hydrogel (Bulkamid) Under Local Anesthesia in the Office: A Prospective Single-center Series. Urology 2025;198():8-13 «PMID: 39580117»PubMed
- Schreiner L, Nygaard CC, Dos Santos TG, ym. Transcutaneous tibial nerve stimulation to treat urgency urinary incontinence in older women: 12-month follow-up of a randomized controlled trial. Int Urogynecol J 2021;32(3):687-693 «PMID: 33057739»PubMed
- Schreiner L, dos Santos TG, Knorst MR, ym. Randomized trial of transcutaneous tibial nerve stimulation to treat urge urinary incontinence in older women. Int Urogynecol J 2010;21(9):1065-70 «PMID: 20458465»PubMed
- Nuotio M, Ala-Nissilä S, Tammela T. Iäkkäiden virtsaamisvaivat ja niiden hoito. Suom Lääkäril 2017;44:2515-2520
- Cilluffo S, Terzoni S, Destrebecq A, ym. Efficacy, effectiveness, usability and acceptability of devices for female urinary incontinence: A scoping review. J Clin Nurs 2023;32(13-14):3361-3377 «PMID: 35851974»PubMed
- Banharak S, Panpanit L, Subindee S, ym. Prevention and Care for Incontinence-Associated Dermatitis Among Older Adults: A Systematic Review. J Multidiscip Healthc 2021;14():2983-3004 «PMID: 34729012»PubMed
- Sosiaali- ja terveysministeriö. Valtakunnalliset lääkinnällisen kuntoutuksen apuvälineiden luovutusperusteet 2023: Opas apuvälinetyötä tekeville ammattilaisille ja ohjeita asiakkaille. https://urn.fi/URN:ISBN:978-952-00-6887-5

